When you receive an antiserum to protect your body from infections, allergy-like symptoms may occur. What is serum sickness? It is a hypersensitivity reaction from an antiserum, certain medications, or injected proteins. Find out more about serum sickness with its explanation.
What is Serum Sickness?
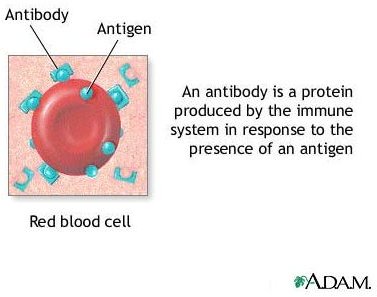
Serum sickness is a kind of a hypersensitivity reaction resulting from an antiserum, certain medications, or injected proteins. The clear liquid of blood is known as serum composed of many proteins such as antibodies, which prevent your body from infection. Antiserum is derived from serum of a person or animal that has immunity or an antibody against a certain microorganism. Your doctor might inject you with antiserum if your body is exposed to life-threatening microorganisms, but your body never receives any immunizations for them. Antiserum you can receive include antiserum for rabies or tetanus. Click on image to enlarge.
Causes
Serum sickness is characterized by a similar response to an allergy in which your body stimulates and produces antibodies to attack a protein from the antiserum because your body falsely assumes it as a danger or antigen. The antibodies and the antigens bind to one another on the layers of cells causing allergy-like symptoms such as inflammation and fever. In addition to antiserum, some medications such as penicillin, sulfa, and cefaclor may result in a comparable reaction.
A reaction may also occur due to particular injected proteins such as rituximab, which is used to cure cancers and immune disorders, and antithymocyte globulin, which is used to treat organ transplant rejection. Blood products from blood transfusions are commonly considered one of the potential causes of serum sickness.
Symptoms
Symptoms usually appear in 7-10 days after exposure but can take as long as 3 weeks. If exposed again, symptoms tend to develop faster (usually 1-4 days). Symptoms that might happen include:
- Joint pain
- Fever
- Hives
- Rash
- Fatigue
- Itching
- Nausea
- Enlarged lymph nodes
- Diarrhea
- Gasping
Diagnosis
Blood tests can reveal problems like blood vessel inflammation. Urine tests can help confirm diagnosis if blood or protein are present and tender and swollen lymph nodes can also indicate serum sickness.
Treatment
If you think you have the above mentioned reactions, inform your doctor right away. Treatments include:
Medications
Your doctor might recommend antihistamines or corticosteroid ointments to treat rashes and itching and/or non-steroidal anti-inflammatory drugs (NSAIDs) such as naproxen and ibuprofen to alleviate joint pain. Your doctor may also suggest oral corticosteroids like prednisone for more severe cases.
Nutrition & Supplements
The following can help support the immune system which can help reduce allergic reactions in general (before taking any supplements, consult with your doctor first):
- Consume a lot of fruits and vegetables
- Consume more lean meats instead of red meats
- Consume omega-3 fatty acids like fish oil
- Consume a lot of water every day (e.g. 7 – 10 glasses)
- Add healthy oils to cooking such as vegetable oil and olive oil
- Take a multivitamin every day
- Avoid trans-fats in foods such as cakes, cookies, French fries, margarine, and donuts
- Avoid food allergens such as dairy milk, soy milk, wheat, chemical additives, and preservatives
- Keep tobacco, coffee, and alcohol at bay
Prognosis
Symptoms normally go away after a few days. Severe reactions can cause anaphylactic shock which can be life-threatening if not treated right away.
References
The University of Maryland Medical Center: Serum Sickness - https://www.umm.edu/altmed/articles/serum-sickness-000149.htm
MedlinePlus: Serum Sickness - https://www.nlm.nih.gov/medlineplus/ency/article/000820.htm
Photo Credit
Image courtesy of the National Library of Medicine.