Medications That Increase Risk of Pressure Ulcers
Introduction
Pressure ulcers develop in bony areas where the patient is bedridden or wheelchair bound. They are caused by constant pressure and friction with sheets or other materials in these positions. Medications that increase the risk of pressure ulcer development include non-steroid anti-inflammatory drugs (NSAIDS) commonly used in the treatment of rheumatoid arthritis.
These risks will be examined further shortly, but first we begin with an overview of pressure ulcers; their causes and treatments.
Overview of Pressure Ulcer Causes
As stated in the introduction, pressure ulcers are prevalent in those people who have been hospitalized and are bedridden, the elderly and infirm being particularly prone. Pressure on the skin from the weight of the body along with friction between the skin and bed sheets are the main causes of pressure ulcers and once manifested, they are very difficult to heal.
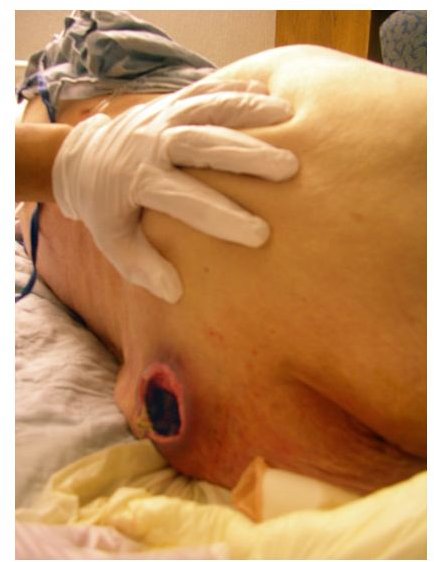
They are usually found in bony locations where the skin is under “point pressure”, and can eventually be so deep as to expose the underlying bone and muscles. The writer has had several rheumatic/vascular leg ulcers where this has actually occurred, being a very painful, debilitating experience.
A typical pressure ulcer and a sketch showing common location of pressure ulcers are shown below; please click on images to enlarge.
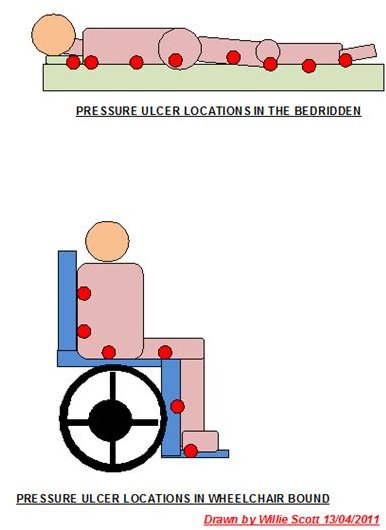
Pressure ulcers can also be caused by medication taken by the patent for other complaints, this will be discussed fully in the next section, meanwhile we look at those at risk of developing pressure ulcers;
- Aged and severely ill.
- Those with poor circulation receiving medication connected with cardiovascular diseases.
- The infirm, bedridden and wheelchair users especially where pain on movement makes them reluctant to change position.
- Patients with rheumatoid arthritis with continual use of anti-inflammatory drugs (NSAIDS).
Treatment of Pressure Ulcers
It is imperative that the pressure ulcers are treated as soon as they appear on the skin; this includes the following treatment.
- Pressure ulcers are extremely painful, especially when they are deep rooted. Pain relief is essential, often strong analgesia being required.
- Provision of a pressure relieving or alternating pressure mattress or cushion, depending on the location of the ulcers.
- An efficient wound management program, including daily dressings and cleansing/ debridement of the ulcers.
Medications That Increase the Risk of Pressure Ulcer Development
The previous section has given an insight into the causes and treatment of pressure ulcers; here the use of certain medicines that increases the risk of ulcer development is examined.
The main medications that increase the risk of pressure ulcer development are non-steroid anti-inflammatory drugs (NSAIDS).
NSAIDS are used to treat the inflamed joints experienced in rheumatoid arthritis.
For many years the author had rheumatoid arthritis and a vascular/rheumatoid leg ulcer, which prevented joint replacement due to risk of infection. This was a catch 22 situation where one needed to take NSAIDS for the joint inflammation, but this inhibited the healing of the ulcer. The answer was to decrease the anti-inflammatory medication and increase the pain relief. The administration from an excellent vascular specialist nurse using modern dressings eventually healed the ulcer; enabling a knee and hip joint replacement within six weeks of each other.
Some common NSAIDS are listed below;
- Aspirin
- Indocide
- Naprosyn
- Volterol (Diclophenic)
- Ibuprofen
These all work in the same way to block cox1 and cox2 inflammatory enzymes, decreasing the swelling and relieving the pain in the arthritic joints.
NSAIDS can increase the risk of pressure ulcer development in the following manner;
- Through hindrance of the chemical activity of arachidonic acid. This is a fatty acid essential for human nutrition.
- Severely restrict platelet function that is required to maintain and develop new skin.
- The development of skin rashes and other detrimental skin effects due to photodermatitis; where the patient is exposed to the sun for too long. This can also lead to skin breaking down and promote pressure ulcers.
Other medications that Increase the risk of pressure ulcer development are;
- Medication such as Nitrazepam and hypnotic drugs to combat sleeplessness also reduce movement; the body remaining in the same position through the night that can cause pressure ulcers.
- The use of beta blockers such as propranolol to control heart problems can cause vasoconstriction, leading pressure ulcers on the feet.
- Blood thinning medication such as Warfarin can cause necrosis; a reddening of the skin leading to lesions and pressure ulcers.
- The use of some cytotoxic drugs and radiotherapy for cancer treatment can affect the skin and cause pressure ulcers.
- Analgesics used to relieve pain can also reduce the need to move about and reduce pressure on the effected areas.
- Inotropes are used to control the heart muscles but can cause vasoconstriction leading to tissue hypoxia; a reduction in oxygen to cell tissues a precursor to pressure ulcers.
References
- Prevention and cures for pressure ulcers: https://www.patient.co.uk/doctor/Pressure-Sores.htm
- Medication and pressure ulcers: https://www.monitor-rx.com/pages/show/common_geriatric_problems
- Effects of NSAIDS and steroids on pressure ulcers: https://emedicine.medscape.com/article/1298452-overview