Oophorectomy Procedure Information
Introduction
An oophorectomy procedure is the surgical removal of the ovaries. During this surgery either one ovary (unilateral oophorectomy) or both ovaries (bilateral oophorectomy) are removed. This surgery may also include removal of the fallopian tubes (salpingo-oophorectomy) or may be done during a total hysterectomy, where the uterus is also removed.
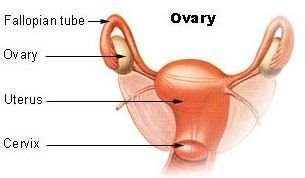
The ovaries are small reproductive organs which contain the eggs necessary for fertilization and produce the hormones needed for a reproductive cycle. Without the ovaries, the levels of the hormones estrogen and progesterone dramatically decrease in the body, and a woman will no longer be able to reproduce. However, if only one ovary is removed, one can still menstruate and have children.
The most common reasons for a surgical oophorectomy include: treatment of ovarian, endometrial, or fallopian tube cancers; removal of ovarian cysts; treatment or prevention of estrogen-reactive breast cancer and/or ovarian cancer; treatment of endometriosis; and treatment of severe premenstrual syndrome.
Before the Surgery
Prior to the oophorectomy, you will likely be given a physical exam, blood and urine tests, and possibly x-rays, a CT scan and/or an ultrasound. Your doctor will discuss with you the risks and benefits of the surgery and why you should opt to have this procedure done. Now is the time to ask any questions you have about the oophorectomy procedure!
A few days before the oophorectomy surgery, your doctor or nurse will advise you on how to prepare for the surgery. These directions may include when to stop eating or drinking before the surgery, when to stop smoking or taking medications before the surgery, and how to plan for your recovery after the surgery.
During the Surgery
During the oophorectomy, you will be placed under either general or local anesthesia, and either one (unilateral oophorectomy) or both (bilateral oophorectomy) of your ovaries will be removed. One of two surgical methods may be used for this procedure: abdominal incision or a laparoscopic procedure.
An abdominal incision surgery is mostly likely performed to remove cancer, as the surgeon can more easily visualize the area. During this procedure a 4-6 inch cut (a little less than the length of your hand) is made either vertically or horizontally through the skin, the abdominal muscles are teased apart, the blood vessels going to the ovaries are tied off, and the ovaries are removed. You are then stitched up and the healing begins.
A laparoscopic procedure for a surgical oophorectomy is less invasive and is usually done for preventative measures or non-cancerous treatment regimens, because it is more difficult to see the ovaries. Here, a small telescope-like device (the laparoscope) is inserted through a small cut (1/4 to 1/2 an inch) in the abdomen. This allows the doctor to view your organs on a T.V. monitor. More small incisions are made to insert small tools to tie off your blood vessels and remove your ovaries. Again, you are stitched up and the healing begins.
After the Surgery
You will feel discomfort or pain after your oophorectomy surgery, but women report less pain after a laparoscopic procedure than an abdominal incision procedure. You will stay in the hospital for a few days after the surgery and, after you leave the hospital, you need to rest and take care of yourself to heal quickly and completely. You should take time off of work, until your doctor tells you it is safe to return to your normal routine.
As with any surgery, there are some risks involved with an oophorectomy procedure, including bleeding, infection, blood clots, and (rarely) death. Make sure you know the warning signs of a problem BEFORE you leave the hospital, which include: fever, chills, heavy bleeding, severe pain, redness and discharge from incisions, and problems with bowel movements or shortness of breath.
After the removal of your ovaries, you will undergo premature menopause. Hormone replacement therapy, if appropriate for your condition, may help relieve these symptoms. Premature menopause may be associated with early onset of osteoporosis, coronary heart disease, elevated atherosclerosis, and depression.
Finally, do not rely on this article as medical advice! ALWAYS consult your doctor for ANY medical advice.
References
[Healthgrades.com](https://www.healthgrades.com/procedures/profile/Ovary_Removal_Surgery_(Oophorectomy)