Treat Anemia in Pregnancy Naturally
Anemia in Pregnancy
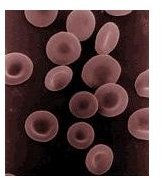
Anemia (low blood iron) refers to a deficit of red blood cells or hemoglobin (iron containing portion of red blood cells) in the blood. Red blood cells are responsible for transporting oxygen from the lungs to the tissues of the body and removes carbon dioxide for excretion by the lungs.
Causes
Anemia may be due specifically to the pregnancy or it may exist coincidentally with the pregnancy. If anemia is not induced by the pregnancy, it can be exacerbated by it. Mild anemia in pregnancy can rapidly become a case of severe anemia.
Although a pregnant woman stops menstruating (conserving iron by not losing blood every month) her body still needs a higher intake of iron for the fetus, the placenta, and her own increased circulating blood volume. The greatest need for increased iron intake is in the second half of pregnancy. With a multiple pregnancy, more iron is needed.
Poor intake of iron is a major cause of anemia. An infection can also be a cause by destroying red blood cells.
Signs and Symptoms
Early signs and symptoms of anemia are listlessness, fatigue, and anorexia.
Late signs and symptoms include pallor, weakness, tachycardia (high heart rate), and palpitations.
Treating Anemia During Pregnancy
Any underlying cause, like an infection, needs to be addressed.
Foods for Anemia
The following foods are rich in iron:
- spinach and other green leafy vegetables
- dried beans
- lean meat
- dried apricots and other dried fruits
- almonds
Beets, sauerkraut, tofu, and blackstrap molasses are other good foods.
Vitamin C greatly enhances the absorption of dietary iron.
Coffee, tea, egg yolk, wheat bran, antacids, and overuse of calcium supplements decrease iron absorption.
Iron Supplementation for Anemia
During pregnancy, it is hard to meet the daily requirements of iron through food.
A prenatal vitamin normally provides enough iron to prevent anemia in pregnancy. If anemic, an iron supplement will also be ordered.
Disclaimer
Please read this disclaimer regarding the information contained within this article.