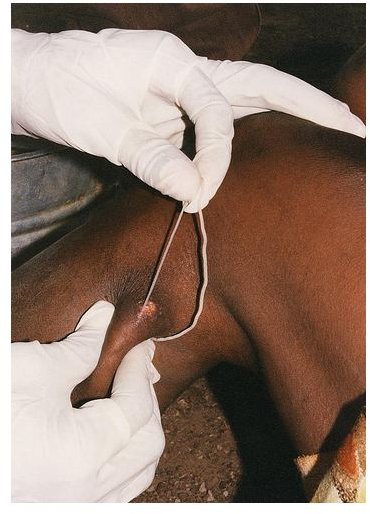
Diagnosis and Treatment of Dracunculiasis
Diagnosis of Dracunculiasis
The absence of obvious symptoms even if D. medinensis parasites (guinea worms) are present in the body is a problem for the early diagnosis of dracunculiasis. The long asymptomatic period is a characteristic of the disease; this demands the development of immunodiagnostic methods for the early detection of the disease. (Bloch and Simonsen 1998)
The first noticeable symptom of the disease is the appearance of a red, itchy papule that rapidly transforms into a blister. According to Rohde et al. (1993), patients who have previous infections become aware of the worm that they can already predict the expected days of the parasite’s emergence. Obtaining samples of juveniles for study can only be done after the blister ruptured. The procedure is done by placing cold water directly to the wound; this stimulates the release of juveniles from the uterus of adult female worms. Then the juveniles are mounted on a slide, they can be seen actively moving under a low-power microscope (Garcia 2001).
The diagnosis of dracunculiasis becomes simple when a part of the worm emerges from the wound. It is however important the worm does not dry out and disintegrate so as to recognize the morphology of the parasite. An intermittent sparganum may de diagnosed as dracunculiasis (Garcia 2001).
Treatment of Dracunculiasis
Pulling out the worms by winding them on a stick has been a popular and successful treatment procedure since antiquity. In addition, the epidemiology and treatment of dracunculiasis is consistent to a biblical account. In the book of Numbers 21:4-8, it said that the Lord sent fiery serpents to the people living near the Red sea; these serpents bit the people with burning pain and killed many of them. The Lord then asked Moses to put three serpents in a pole and place it into an area where the people can see; the bitten people who would look upon the pole will survive. The painful bite of the fiery serpents could be interpreted as the burning pain of the blister and the serpents on the pole could be interpreted as the worms winded off into a stick. As discussed in the part 3 of this series, the life cycle of D. medinensis is usually completed in dry regions like most of the areas near the Red Sea, so it would not be surprising that dracunculiasis became an epidemic at those areas. (Grove 1990)
Try to look on the seal of the American Medical Association. Can you notice the serpent on a staff? Might the staff with serpent depict the removal of guinea worms?

The serpent on the staff is adopted today as the official symbol of medicine. The removal of the worms by winding them on a stick might have been a very popular treatment method in the ancient world that it is not surprising that physicians used it as the ideal symbol for their profession. However, the origin of the symbol and why it was adapted as the symbol for medicine is still a a topic of debate.
Removal of the worms by surgery has been an alternative method of treatment. The surgery is often successful when removing the whole worm near the skin as well as removing worms that were stranded in deep tissues and failed to reach the skin. There are cases when a worm is threaded into a deep fascia or a tendon or is broken into many pieces that it would be impossible to remove completely. Worms can be removed easier and faster if surgery is performed prior to the development of ulcers and the occurrence of

secondary bacterial infections. (Rohde et al. 1993)
According to Muller (1992), various drugs have been used for treating dracunculiasis, but proofs for their efficacy are uncertain.
References
Garcia L. 2001. Diagnostic Medical Microbiology. ASM Press.
Grove DI. 1990. A history of human helminthology. Wallingford, Oxon. UK: CAB International.
Bloch P and PE Simonsen. 1998. Studies on immunodiagnosis of dracunculiasis. I. Detection of specific serum antibodies. Acta Trop. 70:73-86.
Rohde JE, Sharna BL, Patton H, Deegan C, and JM Sheery. 1993. Surgical extraction of guinea worm: Disability reduction and contributons to disease control. Am. J. Trop. Med. Hyg. 48:71-76.
Muller R. 1992_. Guinea worm eradication. Four more years to go_. Parasitology Today 8:387-390.
Photo Credit
https://kids.niehs.nih.gov/pictures/caducea.gif