The Pathogenesis of Dracunculiasis
In part three of this series, we learned the modes of transmission of D. medinensis, now we will explore the facts on how the parasite inflicts illness to human beings. Dracunculiasis may result in three major disease conditions: emergent adult worms, secondary infection by bacteria, and nonemergent worms.
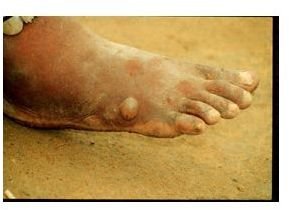
The metabolic wastes produced by female worms migrating in the skin elicit a violent allergic reaction to the host’s system. The reaction triggers the formation of a rash, diarrhea, nausea, dizziness, and localized edema or swelling. For about a month, the worm stays underneath the human skin until a red papule or small bump develops. This papule quickly becomes a blister. The formation of this blister is usually accompanied by extreme burning pain. Although any body surface is susceptible for blister formation, those in the feet and the hands are the ones usually affected. Allergic reactions usually disappear upon the rupture of the blister. The location of the lesion becomes abscessed, but it heals rapidly if no serious secondary infection occurs. Worms usually protrudes at the small holes that remained in the abscessed lesions. Healing of the worm will only be completed if the worms are totally removed or expelled. Unfortunately, infection does not confer immunity to the parasite, and a person can be reinfected many times. (John et al. 2006; Mehlorn and Armstrong 2001; Siew-Yin Long 2001)
Skin abscesses and ulcers are very excruciating and depending on their location and complications, can cause a long period of disability. According to Ogunniyi et al. (2000), about half of cases are complicated by bacterial infection of the ulcers. The pain may be so agonizing that prevents sufferers from leaving their homes or doing any work. The application of antibiotics to the ulcers has been significant in case management.
Worms that protrude out in the tiny holes carry with them bacteria when they retreat. The introduction of bacteria under the skin is the start of complications. In fact, this is the third most common mode of entry of tetanus spores in Africa. Some other complications include abscesses, arthritis, bubo, and synovitis. (Bloch
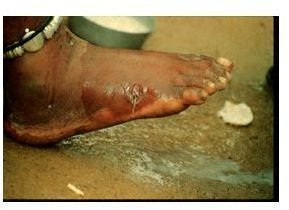
and Simonsen 1998)
In the life cycle of D. medinensis (Garcia 2001), the worms should reach the skin, but there are instances that they fail to reach the skin and stranded in deeper tissues of the body. Many of these worms die and are absorbed or calcified, with no evident effect on human. However, if the worms are calcified alongside the joints, they may cause chronic arthritis. Sometimes the worms enter the central nervous system and cause a serious disease called paraplegia. Adult worms have also been observed in human heart and urogenital organs.
Degenerating worms release antigens that cause aseptic abscesses, which can also lead to arthritis. The abscesses can be huge, holding up to 500 mL of fluid containing leukocytes and often copious D. medinensis embryos.
References
John D, Petri W (contri.), Markell E, and Marietta Voge. 2006. Markell and Voge’s Medical Parasitology. Saunders Elsevier.
Garcia L. 2001. Diagnostic Medical Microbiology. ASM Press.
Mehlorn H and PM Armstrong. 2001. Encyclopedic Reference of Parasitology. Published by Springer.
Fernando RL and A Siew-Yin Long. 2001. Tropical Infectious Diseases: Epidemiology, Investigation, Diagnosis and Management. Cambridge University Press.
Ogunniyi TAB, Oni PO, Juba A, Asaolu SO, and DO Kolawale. 2000. Disinfectants/antiseptics in the management of guinea worm ulcers in the rurals area. Acta Trop. 74:33-38.
Bloch P and PE Simonsen. 1998. Studies on immunodiagnosis of dracunculiasis: Detection of specific serum antibodies. Acta Tropica 70:73-86.
Photo Credit: https://www.dpd.cdc.gov/DPDx/HTML/ImageLibrary/Dracunculiasis_il.htm