Effects of Thyroidectomy on Voice
Thyroidectomy Procedure
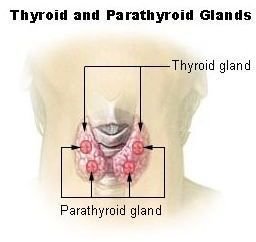
Your thyroid is a butterfly-shaped gland in the base of your neck. The thyroid produces hormones that control your metabolism and affects everything from the rate your heart beats to how quickly you burn off calories.
A thyroidectomy, or surgical removal of your thyroid gland, is used to treat thyroid nodules, thyroid cancer, or hyperthyroidism. During a total thyroidectomy procedure, your entire thyroid gland (both lobes and the narrow band that connects the two lobes, called the isthmus) will be removed. During a partial thyroidectomy, only part of your thyroid will be removed. Partial thyroidectomies can be categorized into subtotal thyroidectomies, where one whole lobe, the isthmus, and most of the other lobe are removed, and a thyroid lobectomy, where only one lobe is removed (with or without the isthmus).
A thyroidectomy is surgery and is usually done under general anesthesia, taking several hours to complete. During a thyroidectomy procedure, a small incision is made in the front of the neck and the thyroid tissue is removed. In some cases, you may have to undergo a tracheotomy during or after the surgery, where a tube is inserted in your trachea to help you breathe.
Effects of Thyroidectomy on Voice
One important concern of patients is how a thyroidectomy procedure may affect their voice after surgery. Both temporary and permanent changes in voice have been well documented following thyroidectomy surgery. Between 16 and 40 percent of patients may have temporary changes in voice soon after a thyroid removal surgery and, by three months post-op, between 2 and 20 percent of patients still complained of complications with their voice. Changes in your voice after a thyroidectomy may include hoarseness, easy fatigue, trouble with high pitches and your singing voice, and decreased voice projection.
Although there is some debate regarding why your voice may be affected by a thyroidectomy surgery, the most common causes include damage to your nerves that control your vocal cord, which are located around our thyroid gland; damage to your strap muscles, which function during talking and singing, or vocal folds; changes in your laryngeal mucosa; or changes in your general condition following surgery. Of these possible causes, damage to your nerves is the most likely to cause permanent changes in your voice.
According to various studies, somewhere between zero and twenty percent of patients have any nerve damage at all, and most studies claim less than 6 percent of thyroidectomy procedures result in nerve damage.
Treatment for Changes in Voice
Interestingly, new studies suggest that treatment with certain steroids prior to thyroidectomy procedures may help improve temporary changes in voice, as well as decrease nausea, vomiting, and pain. This may be worth discussing you’re your doctor prior to surgery.
While permanent thyroidectomy effects on voice are rare, there are some ways to treat this condition. Laryngeal electromyography can give information about how the nerves are working, or aren’t working, to control the muscles of the vocal cords, which allows for a definite diagnosis of laryngeal nerve damage. This procedure, along with vidoestroboscopy, which shows your vocal cords in action, and electroglottography, which measures vocal fold vibrations, can be used to make and accurate diagnosis of the problem.
Laryngeal framework surgery, or thyroplasty, can be performed to try to correct problems resulting from a thyroidectomy procedure. Traditionally, laryngeal framework surgery was performed with the hopes of improving the position of your vocal cords so they vibrate better during speaking or singing. This can be used to repair torn, dislocated, or paralyzed vocal cords by bringing them into a better position for a strong voice.
Recently, a technique called laryngeal reinnervation has opened the field to a new treatment option. Although still in its infancy, this surgical procedure may allow for reinnervation of paralyzed vocal cords damaged during a thyroidectomy in which the laryngeal nerves near the thyroid gland were damaged.
References
Am J Surg. 2007 Sept; 194(3). 317-322.
J Voice. 1997 Dec; 11(4). 479-482.
Arch Surg. 2009;144(2).149-153.
Surgery. 2008 Jun;143(6):732-42.
Clin Anat. 2008 Mar;21(2):99-105
Am J Surg. 2007 Sep;194(3):317-22