What You Need to Know About Bleeding Esophogeal Varices
What are Esophogeal Varices?
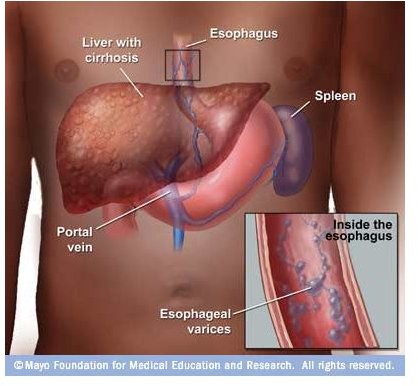
Esophogeal varices are dilated blood vessels in the walls of the stomach or lower esophagus. They don’t usually cause signs and symptoms unless they begin bleeding. The danger occurs when the fragile varices rupture under pressure and bleed. Large blood loss can result in shock and death if not treated immediately.
Esophogeal varices
Causes
Cirrhosis of the liver is the most common cause of esophogeal varices. When the liver is scarred, blood can’t flow through the liver as efficiently, resulting in high blood pressure in the portal vein (portal hypertension). The portal vein carries blood to the liver from the digestive organs. When the pressure increases, blood backs up into the vessels, causing them to swell. Cirrhosis of the liver is most commonly caused by hepatitis or alcohol abuse.
Less commonly, a blood clot in the portal vein can lead to esophogeal varices. Schistosomiasis, a parasitic infection found in South America, Africa, the Middle East, the Caribbean, and Southeast Asia can also cause esophogeal varices.
Signs and Symptoms
There may be no symptoms in people who have chronic liver disease. If only a small amount of bleeding is present, there may be dark streaks in the stools. With larger amounts of bleeding, black, tarry stools or bloody stools, vomiting blood, paleness and light-headedness may be present. The heart rate will be elevated with a low blood pressure.
Tests and Treatments
An esophagogastroduodenoscopy, or EGD, involves passing a lighted scope down to the stomach to look for bleeding. Large varices and those with red streaks have a higher risk of bleeding. CT scans and MRI also detect varices and allow liver function and portal vein circulation to be evaluated. Blood pressure medications such as propranolol may be given to lower blood pressure in the portal vein and prevent bleeding.
If bleeding is present, variceal ligation can be performed to wrap elastic bands around the varices and stop bleeding. Ligation carries the small risk of scarring the esophagus. With injection therapy, a solution to shrink varices is injected into them. This procedure carries the risk of perforation of the esophagus and scarring that can cause difficulty swallowing.
A transjugular intrahepatic portosystemic shunt (TIPS) is a small tube placed between the portal and hepatic veins. TIPS controls bleeding by providing another path for blood. It carries the risk of liver failure and accumulation of toxins in the bloodstream. It is used mainly when other treatments have failed, or the patient is awaiting a liver transplant.
Prognosis and Prevention
Once varices have bled, there is an increased risk of future bleeding and complications. Outcomes tend to be poor. Bleeding can recur, and infection such as pneumonia or peritonitis is a threat. In cases where liver damage is extensive, a liver transplant may become the last option. There are usually many more people awaiting liver transplants than there are donors, and the surgery itself carries many risks.
The best way to prevent bleeding esophageal varices is by maintaining a healthy lifestyle. Do not drink alcohol if you have liver disease. A healthy diet full of fresh fruits and vegetables, with minimal fatty and fried foods may help. Maintaining a healthy body weight and using chemicals safely may stress the liver less. And finally, minimize the risk of hepatitis by not sharing needles and having unprotected sex. Follow your doctor’s advice about the Hep B vaccine.
References
Mayo Clinic: Bleeding esophogeal varices-https://www.mayoclinic.com/health/esophageal-varices/DS00820
Medline: Bleeding esophogeal varices-https://www.nlm.nih.gov/medlineplus/ency/article/000268.htm
Photo Credits
Mayo Clinic-https://www.mayoclinic.com/health/esophageal-varices/DS00820