Alcoholics Seeking Liver Transplants Face Rigorous Screening
Healthy Liver Function
The healthy liver is russet in color and weighs about three pounds. This rubbery organ resembles a rounded-off triangle. The liver detoxifies alcohol, drugs, metabolic byproducts and other poisons from the blood. It manufactures proteins and hormones and converts food into energy.
The Stages of Alcohol-Related Liver Disease
When alcohol is consumed, it produces an inflammatory response in the liver. Over time, this type of inflammation can lead to alcohol-related liver disease, or “ALD”. The three stages of ALD include fatty liver, hepatitis, and cirrhosis.
Alcohol-Related Fatty Liver
Alcohol-related fatty liver is found in 90 to 100 percent of heavy drinkers. A man who consumes 60 grams (four drinks) a day is considered a heavy drinker. In women, heavy drinking is defined as consuming two drinks per day. Women are less tolerant to the effects of alcohol than men, due to differences in body fat distribution and total body weight.
Hepatitis
The second stage of ALD is hepatitis. As inflammation continues, the liver scars and becomes fibrous. It loses its ability to regenerate itself. Beginning signs of hepatitis include fatigue, low-grade fever or nausea. Later symptoms include jaundice, loss of appetite and impaired ability to process nutrients. Hepatitis is irreversible, but if caught early enough, the condition may be managed through medication and by abstaining from alcohol.
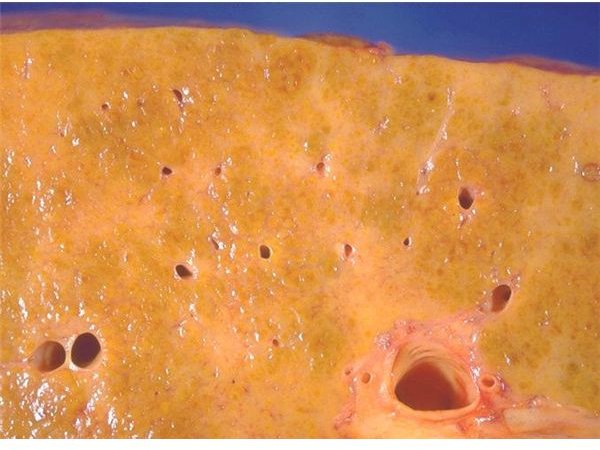
Cirrhosis and Liver Failure
The third stage of alcohol-related liver disease is cirrhosis. Symptoms may include fluid buildup (ascites) in the stomach, gastrointestinal hemorrhage, confusion, change in personality or intellectual capacity, unconsciousness, coma and liver failure.
Ethical Controversy Over Alcoholics and Liver Transplants
This year, over 6,000 people suffering from end-stage liver disease will receive a liver transplant in the United states. More than 1,800 people will die while waiting for a liver transplant. Because there is such a scarcity of donor livers, transplant centers screen all potential candidates for psychosocial and medical risk factors to determine the patient’s eligibility for transplantation. Rehabilitation programs are used to encourage ALD candidates to reduce their risk of alcoholic relapse. Some medical facilities require a six month period of abstinence before they will consider transplantation for alcoholic patients.
Relapse occurs in 16 percent of liver recipients who have a history of alcoholism. Society at large, as well as critics in the medical ethics community, view alcohol-related liver disease as a self-induced “problem”. The implication is that non-alcoholic patients are somehow more “deserving” of a liver transplant than those who have a history of alcohol abuse. The debate continues about alcoholics and liver transplants, and will probably continue as long as there remains a shortage of donor livers and a long list of those waiting for transplantation.
Image Credits
Public domain image of cirrhotic liver scarring, courtesy of Dr. Edwin P. Ewing, Jr., CDC
References
The Merck Manuals Online Medical Library: Cirrhosis - www.merck.com/mmhe/sec10/ch136/ch136c.html
U. S. National Library of Medicine, NIH: The Impact of Acute Alcoholic Hepatitis in the Explanted Recipient Liver on Outcome After Liver Transplantation - www.ncbi.nlm.nih.gov/pubmed/18044757
UptoDate: Ethical Issues in Liver Transplantation - www.uptodate.com/patients/content/topic.do?topicKey=~Go52SvBIB_cwQG