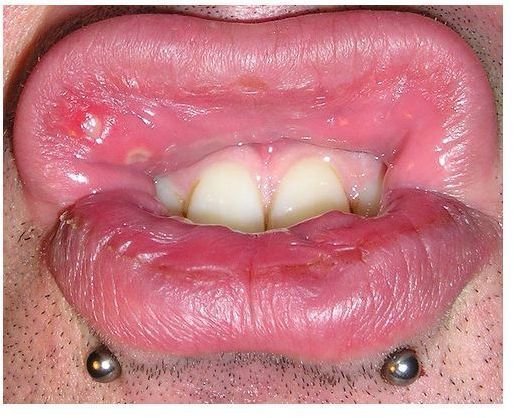
An ulcer is an open sore accompanied by inflammation and or infection, caused by abrasions. Read on to find out more about pressure ulcer vs trauma ulcer, the causes, symptoms, and cures.
A pressure ulcer, also known as pressure sores or bedsores , usually form in the skin in areas where the bone is close to the skin, such as elbows, hips, ankles, shoulders, heels and back. They are usually the result of staying in one position for a long time without shifting the weight. The constant pressure applied on the skin reduces the flow of blood, causing the death of tissues and ultimately forming ulcers. This type of ulcer starts as reddened skin, and gradually advances into a blister, an open sore and eventually a crater. Trauma ulcers occur in the mouth and are the result of injuries to the oral cavity from inadvertently biting oneself when talking, eating, or sleeping, misfit dentures, malformed or jarred teeth, shocks, and other faulty oral hygiene causes that cause formation of surface ulcerations. If these ulcers fail to heal after two weeks of treatment, they can develop into oral cancer. Image Credit: Wikimedia Commons
Causes and Prevention of Pressure Ulcer vs Trauma Ulcer
The following conditions increase the risk of developing pressure ulcers:
-
- bedridden or wheelchair-bound for any length of time
- spinal or brain injury that may cause disability
- diabetes or vascular disease that prevents proper blood flow to the skin
- fragile skin
- malnourishment
- old age that restricts movement of body parts
- urinary or bowel incontinence
- mental disability from conditions such as Alzheimer’s disease that prevents the patient from taking preventive steps
The best way to prevent pressure ulcers is to pre-empt the causative factors. Some pointers in this direction include:
-
- changing position at frequent intervals, about every two hours and using pillows, sheepskin, foam padding, and powders when bed-ridden or incapacitated
- eating well-balanced meals and drinking about 8 to 10 glasses of water a day
- keeping skin clean and dry
The following conditions rank among the most common causes of trauma ulcer:
-
- dental symptoms such as fractured, carious, malposed, or malformed teeth, or premature eruption of teeth
- xerostomia or dry mouth
- Ill-fitting dentures
- fractured jaw
- accidentally biting oneself while talking, sleeping or eating
- consumption of very hot foods
- eating food with rough edges
- mechanical trauma
- electrical shocks, especially to young children
- exposure to harmful chemicals such as aspirin, hydrogen peroxide, silver nitrate, and phenol that causes damage to the oral mucous membrane
- nocturnal parafunctional habits such as grinding teeth and thumb sucking
Trauma ulcers are mostly the result of accidents, and the best way of prevention is taking care to prevent the accidents, and by ensuring that dentures fit correctly, problems with the teeth are resolved early, food is not consumed very hot, consuming plenty of water to prevent dry mouth, and other similar precautions. Sometimes patients with psychological symptoms self-inflict themselves with trauma ulcers to seek medical attention.
Continue to page 2 for symptoms and treatment options for pressure ulcer vs trauma ulcer
Symptoms of Pressure Ulcer vs Trauma Ulcer
Pressure ulcers symptoms depends on the stage of the ulcer. Pressure ulcer develop in four stages, ranked by severity and distinguished by appearance
-
- Stage I, or the earliest stage, manifesting as a reddened area on the skin that when pressed does not turn white
- Stage II or blisters and sores with red and irritated skin
- Stage III when the skin breaks down causing damage to skin tissues, and the ulcer resembles a crater
- Stage IV or the most advanced stage when the ulcer becomes very deep to cause damage to muscles, bones, tendons, and joints
Trauma ulcers occur throughout the oral cavity. Self-inflicted ulcerations such as accidental biting most commonly occur on lips, tongue, and inside the cheeks, and ulcerations caused by foreign objects most commonly occur in the palate or roof of the mouth and gums. Trauma ulcers resultant from mechanical trauma and electrical shocks usually manifests in the upper and lower lips and the lateral border of the tongue, and ulcers resultant from consumption of hot foods usually occurs on the inside the cheek and on the palate. Trauma ulcers usually manifest as erythema or areas of redness surrounding a central, yellow, membrane comprised of fiber and puss, but may have varying features depending on the cause. Sometimes, a rolled border develops adjacent to the ulceration.
Treatment
The immediate cure for pressure ulcer is to relieve the pressure on that area and avoid further friction by using pillows, special foam cushions, and or sheepskin, or by changing the position. Treating pressure ulcers starts when the ulcers advance from blisters into open sores, and include opening and cleaning the ulcer using salt-water to keep the area clear of dead tissues to prevent infections, and covering the ulcer with gauze. Pressure ulcers require medical help only when it the skin breaks down and the ulcer advances into a crater, posing risk to the muscles and bones, or when inflection starts to develop. The earliest signs of inflection include foul odor from the ulcer, redness, warmth, swelling, and or tenderness around the ulcer. Fever or weakness is a sign of the inflection having spread to the blood or other parts of the body. The treatment options for trauma ulcer depend on the size, duration, and location of the ulcer. Treatment options for minor ulcerations include removal of the irritants such as ill-fitting dentures, use of a soft mouth guard or sedative mouth rinse, application of topical corticosteroids or anesthetics, and or switch over to a soft and bland diet. Most trauma ulcerations resolve by itself within 10 to 14 days and the best treatment option is removal or prevention of the obvious cause. Severe and deep-seated ulcerations may require vaccine, and antibiotics to prevent infection.
References
-
- University of Maryland Medical Center. “Pressure Ulcer.” https://www.umm.edu/ency/article/007071.htm Retrieved 26 November 2010
- Medicine Plus. “Pressure Ulcer.” https://www.nlm.nih.gov/medlineplus/ency/article/007071.htm . Retrieved 26 November 2010
- Houston, Glen. “Traumatic Ulcers.” https://emedicine.medscape.com/article/1079501-overview . Retrieved 26 November 2010.
- WrongDiagnosis. “Trauma Ulcer.” https://www.wrongdiagnosis.com/symptoms/trauma _ulcer/treatments.htm. Retrieved 26 November 2010.