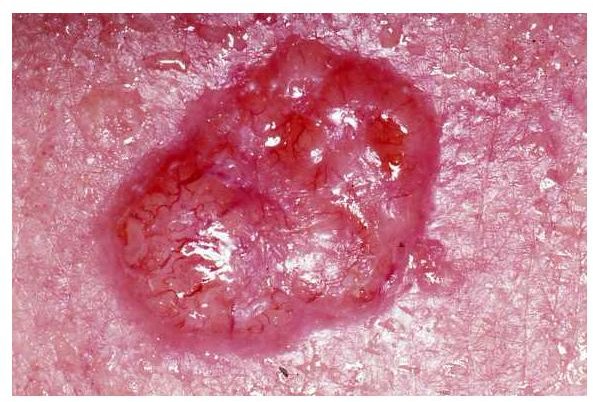
Are you going through treatment for basal cell carcinoma? If so, read on to learn more about the basal cell carcinoma surgery treatments available.
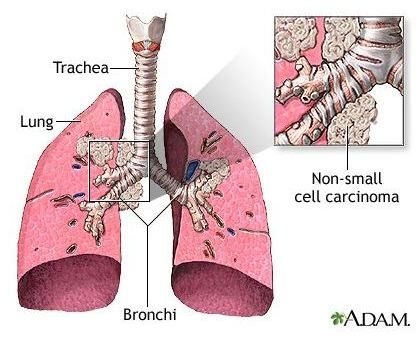
Basal cell carcinoma is a type of non-melanoma skin cancer, and it is also the skin cancer that is the most common. This type of skin cancer is least likely to spread, is the most easily treated, and is rarely fatal. However, there is a high recurrence rate, and people who have had this cancer must often battle it again within five years. If this cancer is not removed, it can cause extensive damage to the tissue and bone that surrounds it. Various types of basal cell carcinoma surgery are the most common ways to remove this cancer.
What Causes Basal Cell Carcinoma?
Long-term exposure to sunlight’s ultraviolet radiation is the most common cause of this type of skin cancer . Other environmental factors include therapeutic radiation, immunosuppressant drugs, and chemical toxins. Genetic factors include nevoid basal cell carcinoma syndrome, xeroderma pigmentosum, and Bazek’s syndrome.
Electrodesiccation and Curettage
After the patient is adequately anesthetized, a curette is used to scrape the tumor. Then, the lateral margins and base of the tumor are electrodesiccated. This is done two times. Electrodesiccation controls bleeding and destroys cancer cells through the use of an electric current.
The advantage of this procedure is that it takes less than five minutes to complete and it is quite effective in treating superficial and primary nodular basal cell carcinoma, with up to 95 percent of patients being cured.
The disadvantages will depend on the surgeon. It is less effective than Mohs micrographic surgery for most types of this cancer, less effective on the nose, and patients will usually be left with a white atrophic scar.
Curettage without Desiccation
This basal cell carcinoma surgery is done in the exact fashion as electrodesiccation and curettage, except no electrodesiccation is done. The advantages and disadvantages are also the same.
Curettage with Erbium
This surgery is done like all other curettage scraping, however, the the ulcer that forms afterward is then ablated along with a one millimeter margin of bordering epidermis. This is often done twice.
This surgery takes less than five minutes, has the same cure rate as other curettage methods, and some feel the cosmetic is more favorable than electrodesiccation.
The disadvantages are nearly the same as all other curettage procedures.
Surgical Excision
This surgical method is done, once adequate anesthesia has been given, to cut down to the subcutis. Skin that appears normal must also be excised in order to ensure all affected skin (clinically invisible tumor extension) is removed. Most patients will have a three to four millimeter margin of normal clinically uninvolved skin excised. This procedure is usually done at the same time as a skin biopsy.
This surgery has an estimated 95 percent cure rate and cosmetic results that are good to excellent.
The results are ultimately dependent on the surgeon. Disadvantages include being not nearly as effective in treating recurrent forms of this cancer and being less effective in treating tumors that do not have clinical margins that are clearly defined.
Mohs Micrographic Surgery
During this surgery, excision or curettage is used to remove clinically apparent tumors, once adequate anesthesia is given. During this procedure the surgeon will begin by removing a thin layer of tissue and will continue to remove thin layers until all abnormal cells are gone. As each layer is removed, it is analyzed under a microscope to determine whether it is abnormal or unhealthy.
This surgery has the highest cure rate, the lowest recurrence rate, and spares as much healthy skin as possible.
The disadvantages include this surgery being time-consuming, not widely available in some areas, it is expensive, and patients may need to have additional anesthesia before each layer of skin is removed.
Cryosurgery
This type of surgery is performed by applying liquid nitrogen directly to the clinically apparent tumor. At the lateral margin, a temperate probe is then placed into the skin. Once the lateral margin temperature reaches negative sixty degrees Celsius, treatment stops. This treatment is rarely used for this type of skin cancer and patients an experience some swelling and pain in the area once it thaws.
The advantages include good cosmetic results, good cure rates when the clinical margins are well-defined, and this is a good option for patients in which surgery is not a good option.
The main disadvantage is that the effectiveness of treatment is highly dependent on the surgeon accurately detecting the clinical tumor margins.
Laser Surgery
This procedure uses lasers with high-energy rays. The carbon dioxide laser will stop cancer growth and damage cancer cells. This is a good option for patients who have superficial basal cell carcinoma and have a high bleeding risk. After the procedure, patients may experience some skin changes that can last for several years.
Resources
Bader, R.S. MD, et al. (2009). Basal Cell Carcinoma. Retrieved on June 15, 2010 from Medscape: https://emedicine.medscape.com/article/276624-overview
Mayo Clinic. (2009). Basal Cell Carcinoma. Retrieved on June 15, 2010 from the Mayo Clinic: https://www.mayoclinic.com/health/basal-cell-carcinoma/DS00925
Image Credits
Basal Cell Carcinoma: John Hendrix MD – Wikimedia Commons