This article (part 2 of the series) presents the morphoanatomy and life cycle of a medically important parasitic nematode: D. medinensis.
Morphology of Dracunculus medinensis
Dracunculus medinensis (Mehlorn and Armstrong 2001; Matthews 1998) is one of the biggest nematodes known. Adult females can reach a maximum length of up to 800 mm long, but males can only reach a maximum length of 40 mm. The mouth is tiny and has a triangular shape and is enveloped by a sclerotized, quadrangular plate. Lips are not present. The cephalic papillae are arranged in an outer circle of 4 double papillae at about similar level as the amphids and an inner circle of 2 double papillae, which are unique in that they are dorsally and ventrally located. A huge glandular portion is located at the esophagus and it protrudes and lies at the side of the thin muscular portion.
Biology of Dracunculus medinensis
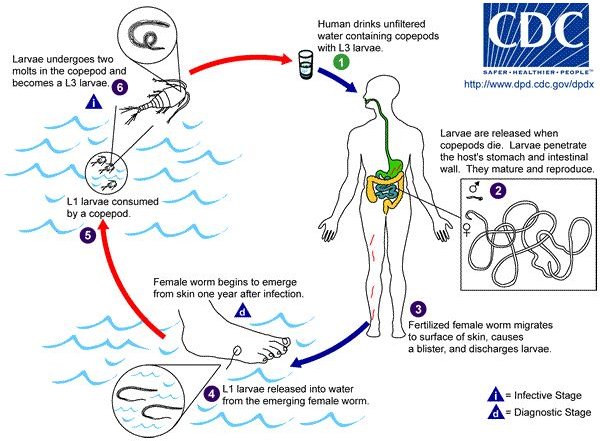
Ovoviparity is a characteristic D. medinensis. The thousands of embryos in the uteri of a gravid female produce high internal pressure. At this phase of the life cycle, it has migrated to the host’s skin. The lower limbs of the host’s body are the most likely to be infected, but any body portion is susceptible for infection (Okoye et al. 1995). When the worm’s uterus and body wall burst because of the high internal pressure, the juveniles are freed into the host (human). The release of the juveniles initiates violent allergic reactions that cause the formation of skin blisters in the host. These skin blisters eventually rupture, creating an exit for young worms which trickle out onto the host’s skin. In some instances, instead of the body wall rupturing, the uterus forces itself out of the parasite’s mouth. The contracting body wall muscles of the host force juveniles out in periodic spurt, with more than 500,000 expelled at a single time. Cool water instigates the contraction of the muscles, which causes the worm and its uterus to protrude through the wound. When portions of the protruding uterus are emptied of their juvenile contents, they disintegrate, and adjacent portions move into the ulcer or rupture. Healing of the wound happens only when the entire worm is “used up”. (John et al. 2006; Cox 1993)
The freed juveniles (J1s) must directly enter water in order to survive. They can live 4 to 7 days but are able to infect an intermediate host (crustacean) for only 3 days. For the juveniles to develop further, they must be ingested specifically by a cyclopoid crustacean (e.g. Cyclops vernalis). Upon reaching the intestine of the crustacean, the juveniles penetrate into the hemocoel, especially below the gut, where they develop into infective J3s within 12 to 14 days at 25 degrees Celsius.
Definitive hosts (humans) are infected by ingesting infected copepods with drinking water. Freed juveniles break through the duodenum, cross abdominal mesenteries, perforate the abdominal muscles, and enter subcutaneous connective tissues, where they move to inguinal and axillary regions. The 3rd molting of the parasite occurs about 20 days after infection, and the last one at about 43 days. Males fertilize the females by the 3rd month of infection; and between the 3rd and 7th months, become encysted and eventually degenerate. The gravid females travel to the host’s skin between the 8th and 10th months, by which time the embryos are fully developed. Ten to 14 months after the initial infection, the female worm causes skin blister. A person with the blister usually experiences intense burning pain, but immersing the wound into the water somewhat alleviate the pain. (John et al. 2006)
Life Cycle of D. Medinensis
References
- Cox F. 1993. Modern Parasitology: A Textbook. Blackwell Publishing.
- John D, Petri W (contri.), Markell E, and Marietta Voge. 2006. Markell and Voge’s Medical Parasitology. Saunders Elsevier.
- Matthews B. 1998. An Introduction to Parasitology. Cambridge University Press.
- Mehlorn H and PM Armstrong. 2001_. Encyclopedic Reference of Parasitology_. Published by Springer.
- Okoye SN, Onwuliri COE, and JC Anoside. 1995. A survey of predilection sites and degree of disability associated with guinea worm (Dracunculus medinensis). Int. J. Parasitology. 25:1127-1129.
Image Credit: United States Centers for Disease Control (https://www.dpd.cdc.gov/DPDx/HTML/Dracunculiasis.htm )