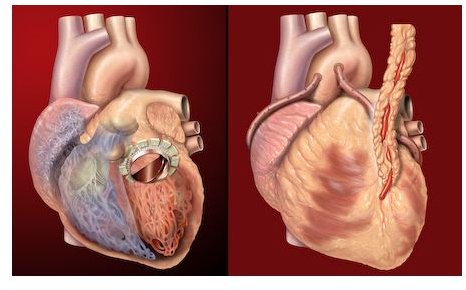
Coronary artery plaques are the result of high cholesterol levels which put a person at risk for death due to heart disease. Learn more about treatment with high dose statins to reduce coronary artery plaque which has been found to be effective in decreasing the risk for heart attack and death.
What Are Coronary Artery Plaques?
The arteries supplying blood to the heart are called coronary arteries, and when cholesterol builds up within them plaques are formed. These harden and decrease the diameters of these vessels, resulting in a compromised blood and oxygen supply to the heart. With time the heart muscles fail, and a heart attack may ensue, leading to death if not treated immediately.
The body produces cholesterol for building cells using fats in the diet. However, there are LDL cholesterols which are bad, and there are HDL cholesterols which are essentially good, in that they help in the removal and excretion of the bad cholesterol. Too much cholesterol production may result from a high fat diet, and these fatty substances may be deposited around organs and inside blood vessels, a condition called atherosclerosis.
How Do Statins Work?
Patients are usually advised to modify their diets to decrease fat intake and increase fibers that facilitate fat removal from the body. However, when these do not work in significantly decreasing blood cholesterol levels and the patient is in danger of complications from heart disease, medications are recommended.
Statins are powerful drugs that reduce bad cholesterols by blocking its synthesis and causing reabsorption of fat build-up on the arterial walls. They also increase the levels of good cholesterol (HDL cholesterol), thus aiding in elimination of the plaques from the arteries.
Popularly prescribed statins like atorvastatin (Lipitor), fluvastatin (Lescol), lovastatin (Altoprev, Mevacor), pravastatin (Pravachol), rosuvastatin (Crestor) and simvastatin (Zocor) have been used to treat atherosclerosis, but until recently they have only been shown to slow down its progression.
The Use of High Dose Statins to Treat Atherosclerosis
Statins are usually given at 5 to 80 milligrams dosage, depending on the kind of medication and level of blood cholesterol. These drugs are usually prescribed if one’s total cholesterol level is 240 mg/dL, (6.22 mmol/L) or higher, or if the LDL level is 130 mg/dL (3.68 mmol/L) or higher. Lower doses are given if the blood cholesterol levels are not too high.
Persons who are suffering from atherosclerosis and at the same time have other risk factors like hypertension , diabetes, obesity, heart disease and poor general health may be given higher doses. Studies have shown that treatment with high dose statins to reduce coronary artery plaque can decrease the risk for heart attack and stroke significantly instead of just slowing down the process of atherosclerosis.
However, there are some concerns on the potential risks of using high doses of statins. These side effects, although unusual, include:
- Abnormalities in liver function tests, indicating liver damage.
- Inflammation of the muscles, called myopathy, where one experiences muscle pains.
- Rhabdomyolysis may occur, where the muscle cells break down and release proteins into the blood and pass out the urine. This is dangerous to the kidneys, because the proteins can damage kidney cells. Statins may also interact with other drugs the patient may be taking, such as gemfibrozil, erythromycin, antifungal medications, nefazodone, cyclosporine and niacin, leading to rhabdomyolysis.
The safe use of high doses of statins requires medical supervision. Aside from computation of doses, precautions in taking statins with other medications should be observed. It is also recommended that liver function tests should be done six weeks after the start of intake of these medications and then regularly after continuous statin therapy. This is because side effects may not be manifested in symptoms and may only be detected by laboratory examination.
References
Circulation, “Statins: Powerful Drugs for Lowering Cholesterol: Advice for Patients” accessed 1/12/11
https://circ.ahajournals.org/cgi/reprint/105/13/1514
Mayo Clinic, “Statins: Are these cholesterol-lowering drugs right for you?” accessed 1/12/11
https://www.mayoclinic.com/health/statins/CL00010
UK Health Care, “High-intensity statin therapy found to reduce plaque in heart arteries” accessed 1/12/11
https://ukhealthcare.uky.edu/publications/AI/cardio/statin.htm