Occlusive arterial disease is a general term for any condition that causes a blockage of arteries in any part of the body. It can be a serious disorder because a block in circulation can lead to complications including organ failure and death.
The Arteries
Arteries are blood vessels that conduct blood from the heart to the different parts of the body. The aorta, the largest artery which comes directly from the heart, branches out into smaller peripheral blood vessels supplying all organs, including the extremities (arms and legs) and the brain.
Arteries are elastic vessels that have muscular walls that can pump and contract to propel blood to deliver oxygen and nutrients to the different areas of the body. Many diseases can affect the arteries, causing their diameters to decrease and cause a limitation in blood flow. When these vessels become occluded or blocked, failure of oxygen delivery will lead to damage and eventual death of tissues.
The Role of Atherosclerosis in Occlusive Arterial Disease
Accumulation of fat on the walls of arteries causes them to harden and decrease in diameter. This condition is called atherosclerosis, and affects about one-third of adult Americans. Over time, obstruction to blood flow in tissues causes symptoms to develop, and if severe, may lead to ischemia or damage. The fatty deposits or plaques can also get dislodged and form a thrombus which can mechanically cause a complete obstruction to blood flow, leading to death of cells and tissues.
Risk factors in developing occlusive arterial disease are advanced age, diabetes, obesity, hypertension, family history of atherosclerosis, high blood cholesterol, smoking and a sedentary life style. Although the exact mechanisms are unknown, smoking is the greatest risk factor associated with arterial disease.
Atherosclerosis is a systemic disease affecting the whole body but certain parts of the body may be more affected than others. Therefore, arterial occlusion can be found prominently in specific areas as shown below.
Peripheral Arterial Occlusive Disease
When atherosclerosis affects arteries of the body, excluding those of the heart and brain, it is commonly referred to as Peripheral Arterial Occlusive Disease (PAOD) or simply Peripheral Arterial Disease (PAD). When the condition affects the lower extremities or legs, it is referred to as Lower extremity arterial occlusive disease. Although symptoms may be prominent in the lower extremities or other body areas, narrowing of arteries may occur at the same time in other areas like the heart and brain, too.
Many people have no symptoms initially, but at the other end of the spectrum there is severe leg pain or intermittent claudication, which is the most distinctive mark of PAD. This usually occurs when the patient is walking, but can also occur at rest. The legs are usually cool because of the lack of blood circulation, and there can be darkening of the skin and ulceration.
When the blood supply to the kidneys is affected, then the condition is called renal artery occlusive disease. Mesenteric artery occlusive disease on the other hand involves the blood supply to the intestines.
Lack of blood supply to the kidneys will manifest initially as uncontrolled blood pressure. If untreated, it will eventually lead to kidney failure.
In the intestines the disease is manifested as loss of weight, severe abdominal pain, obstruction to food passage and gangrene or death of the intestinal tissues.
Carotid and Cerebral Artery Occlusion
The carotid artery is the main arterial supply to the brain. Networks of smaller arteries also form to supply the different areas of the brain which controls motor and sensory functions of the body. A decrease in the blood supply to the brain due to atherosclerosis can bring about headaches, fainting, seizures and stroke. A stroke may bring about weakness, paralysis or sensory deficits, depending on the extent and area of the brain affected. Other effects on the brain may include amnesia, epilepsy and migraines.
When a large area of the brain is affected edema or swelling can take place, thus increasing the pressure inside the skull. If left untreated, this can lead to death.
Coronary Artery Occlusive Disease
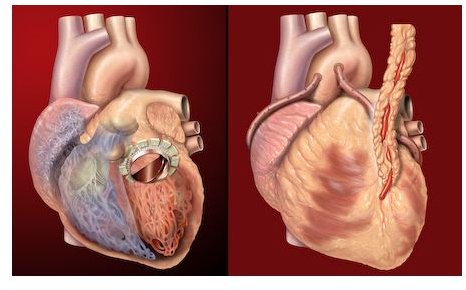
Occlusion of the arteries supplying the heart muscles is the cause of chest pains or angina, and this can lead to a fatal heart attack. Risk factors that are associated with coronary artery disease are similar to those of atherosclerosis in other parts of the body. However, since the heart muscles do not regenerate, just like those of the brain, a severe or complete block to its blood supply can be fatal within minutes.
Diagnosis of Occlusive Arterial Disease
Complete history, physical examination and laboratory work-up are extensively done to evaluate the condition of the patient and the extent of tissue damage involved. Blood and urine tests, ECG and imaging exams are done for initial screening.
Tests usually reveal an elevated blood cholesterol level, abnormal levels of blood sugar, high blood pressure, sugar and/or albumin in the urine, abnormal ECG readings, abnormal liver function test results and others, depending on the main organs affected.
More specific tests include Doppler ultrasound, angiography and arteriography to evaluate blood as it flows through the blood vessels. Depending on the organs involved, other tests may be done to diagnose the disease.
Treatment of Occlusive Arterial Disease
Prevention and treatment of atherosclerosis are essential to managing the disease. Risk factors that can be modified should be given attention, such as:
- Stop smoking
- Follow a healthy diet and maintain an ideal body weight.
- Exercise regularly, avoiding a sedentary lifestyle.
- Manage other conditions such as blood sugar and cholesterol levels, blood pressure and other disease.
Definitive treatment includes:
- Drugs to decrease cholesterol levels such as statins, treat hypertension and diabetes
- Aggressive pharmacotherapy to treat thrombosis or blood clotting, like heparin injections and other oral anticoagulants
- Surgical revascularization to create new passageway or bypass for more blood flow
References
Yonsei Med J, “Antiphospholipid Syndrome and Vascular Ischemic (Occlusive) Diseases: An Overview” accessed 12/20/10
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2628175/
The Internet Journal of Surgery, “Management of Peripheral Arterial Disease: An Overview” accessed 12/20/10
https://www.ispub.com/journal/the _internet_journal_of_surgery/volume_8_number_1/article/management_of_peripheral_arterial_disease_an_overview.html