Those that have suffered from aortic valve stenosis in the past and undergone a valve replacement can endure complications with artificial aortic valve stenosis. This article provides an overview of this disease including symptoms, how its diagnosed, and treatments available.
Anatomy of the Heart: Role of the Aortic Valve
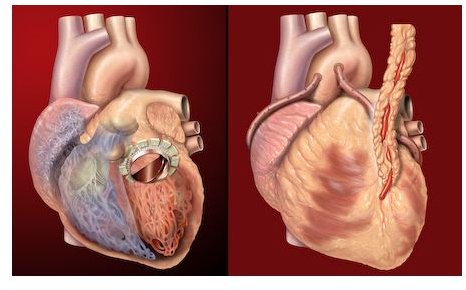
The heart contains four chambers and four valves. One such valve, the aortic valve, is located in the left lower chamber. This special valve allows the blood to flow from the left ventricle to the aorta, a rather large blood vessel. From here the blood is distributed throughout the body, carrying oxygen and essential nutrients necessary for survival.
These valves assist in prolonging life; however, they may be succumbed to a number of aortic valve diseases. When this occurs, an individual may receive an artificial aortic valve implant made from either an animal, human or synthetic material. Along with an artificial valve may come a host of complications.
What is Artificial Aortic Valve Stenosis?
One such complication is a disease known as artificial aortic valve stenosis. The aortic valve becomes narrow, creating an obstruction to the blood flow. Thus, the heart must work hard to force the blood through the aortic valve. After a period of time, the heart grows tired, leading to heart failure. This typically affects patients with valves made from either human or animal materials versus synthetic.
Possible Symptoms Associated with Artificial Aortic Valve Stenosis
Patients will more than likely remain asymptomatic until the condition is severe. At this point, the patient will experience obvious symptoms, including one or all of the following:
- Arrhythmia (irregular heartbeat)
- Tachycardia (rapid heartbeat)
- Angina (chest pain)
- Loss of consciousness
- Fainting
- Dizziness
- Chest discomfort
- Heart palpitations
Artificial Valve Stenosis is Diagnosed Through Various Medical Tests
A heart murmur is indicative of this condition. It may be heard by a health care provider through a stethoscope. There are an array of tests to give a definitive diagnosis, such as an echocardiogram, stress echocardiogram (stress test), electrocardiogram, chest x-ray, brain natriuretic peptide test, cardiac catheterization, and coronary angiogram.
Surgical Intervention is Inevitable for Those with Artificial Aortic Valve Stenosis
Surgery to remove and replace the artificial valve is generally the first course of recommended action for those with severe stenosis. Without surgery, heart failure or death may occur within five years. Those that are unable to undergo open heart surgery to increase the size of the valve opening through a balloon valvuloplasty,
Artificial valves are not curative. According to eMedicine in their article Prosthetic Heart Valves by Gian M. Novaro, “a prosthetic heart valve commits a patient to continued infective endocarditis prophylaxis, regular cardiac follow-up, and often continued medical therapy….”[2] Medications are often used to treat or relieve symptoms; however, they also do not provide a cure.
Patients with Artificial Aortic Valve Stenosis May Be Monitored
If symptoms are not present, it is possible to avoid urgent surgical intervention. Patients will need to be closely monitored by their physicians, however. If at any time symptoms appear, they need to contact their doctor immediately.
Mild artificial aortic valve stenosis may be monitored at different intervals with an echocardiogram. The lesser the severity, the greater the length of time between tests. For instance, suggested observation echocardiogram schedule for mild stenosis may be every three to five years, moderate every one to two years, and severe every six to twelve months.
References:
1. CIGNA website. Aortic Valve Stenosis . Accessed December 3, 2010.
2. eMedicine website. Prosthetic Heart Valves . Accessed December 7, 2010.