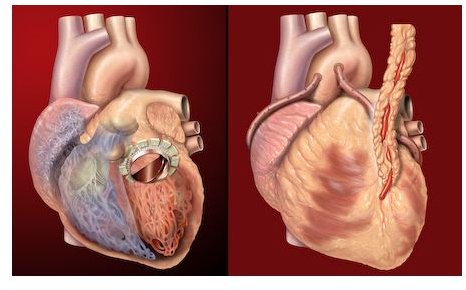
Heart failure often develops in patients with severe defects in their mitral valves. This necessitates either valve repair or replacement when medications do not work. Complete relief of symptoms often results from surgery, but what are the complications of mitral valve replacement?
What is Mitral Valve Replacement?
The mitral valve is a two-leaf flap that guards the opening on the left ventricle, which is the lower chamber of the left side of the heart. Oxygenated blood from the lungs goes to the left atrium which then contracts to push blood across the valve to the ventricle below it. The mitral valve acts to prevent backflow of blood from the ventricle to the atrium when its muscles pump the blood to the general circulation.
When the mitral valve fails to open or close completely due to congenital or acquired disease, symptoms of heart failure will eventually result unless the disorder is resolved. It can be surgically repaired when medications cannot treat the symptoms, but when the valve is severely damaged by disease, it has to be replaced.
The mitral valve may be replaced with a biological tissue valve which can come from a pig, cow or human cadaver donor, or with a mechanical valve made of metal, cloth or ceramic.
Mechanical valves can last a lifetime and are ideal for young patients. However, blood clots may form around or near the valves so that medications to prevent clotting (anticoagulants) have to be taken for life. Women in their child-bearing age are not advised to have these if they plan to have children since anticoagulants can cause fetal birth defects.
Biological tissue valves do not result in blood clotting and anticoagulants are not indicated; however, they are subject to deterioration and for patients who are below the age of 50, reoperation or another replacement may have to be done when this occurs, usually after 12-15 years.
Mitral valve replacement is done under general anesthesia. It may be done under open chest surgery, where the breast bone is split, or under minimally invasive conditions using small incisions and computers. During open chest surgery it will be necessary to keep the patient attached to a heart-lung bypass machine for a certain duration when the heart is paralyzed to allow for surgical manipulation while maintaining circulation and respiration.
Complications of Mitral Valve Replacement
After replacement of a defective heart valve the patient usually experiences a dramatic relief from symptoms of heart failure . However, a few risks exist and complications may occur. It is important to emphasize that although these are possible, modern technology and advances in surgical, medical techniques and nursing care lessen their probability.
General anesthesia poses some risk for complications as in any surgery. These include:
- Hypersensitivity and idiopathic reactions to the anesthesia
- Arrhythmias (irregularities in heart rate and rhythm)
- Breathing problems
Complications related to the use of a heart-lung bypass machine include:
- Arrhythmias
- Heart attack
- Stroke
- Kidney failure
- Pneumonia
- Death
Complications related to surgery include:
- Generalized infection which is common in diabetics and the obese
- Bleeding which necessitates blood transfusion
- Severe postoperative pain
- Reactions to medication
- Infection of the valve
- Thrombosis or formation of blood clots
- Stroke
- Renal failure which necessitates dialysis
- Scarring
- Post-pericardiotomy syndrome, which consists of low grade fever and chest pains lasting for a few to several months
- Memory loss or “fuzzy thinking”
- Failure of the valves to function (rare)
In some instances prolonged antibiotic intake, repeat surgery and prolonged hospital stay might be required. It is rare that permanent disability or death will result unless the condition of the patient is serious. Young patients have less than 5% risk of mortality after the procedure, while older patients who have pulmonary hypertension and other medical problems have an increased risk of death. The five-year survival rate of patients after mitral valve replacement is around 80%.
References
Medline Plus, “Mitral Valve Surgery - Open “, accessed 1/17/11
https://www.nlm.nih.gov/medlineplus/ency/article/007412.htm
Encyclopedia of Surgery, “Mitral valve replacement” accessed 1/17/11
https://www.surgeryencyclopedia.com/La-Pa/Mitral-Valve-Replacement.html