Many people are not aware that tumors can grow from hair follicles in the skin. Most of these tumors are non-malignant but occasionally some can develop to become cancerous, such as the malignant proliferating trichilemmal tumor. Learn more about this rare tumor that grows mostly in the scalp.
Pilar Cysts and Trichilemmal Tumors
Fluid-filled new growths or cysts are common in the skin, scalp and its associated structures like hair follicles and glands. These new growth are called cutaneous cysts, and when associated with the outer root sheath (covering) of a hair follicle, they are called pilar cysts.
Pilar cysts are commonly found in 5 to 10% of the population, and they usually occur in the scalp where hair follicles abound. They are also characteristically seen in older women, and may arise due to inflammation of trauma. Almost all of them are benign or non-life threatening. However, in rare cases (2 percent) they grow rapidly and become proliferating trichilemmal tumors.
The name may sound intimidating, but “trichilemmal” just refers to the hair follicle in more scientific terms. These are still benign and localized, but when they transform to a more aggressive cell growth and appearance changes, they become more abnormal, and are now considered cancerous or malignant. Thus, the term malignant proliferating trichilemmal tumor (MPTT) refers to a cancerous tumor of the hair follicle.
Malignant Proliferating Trichilemmal Tumor
In essence, therefore, the rare MPTT occurs in middle aged and older women, has no racial predilection, and usually begins as a benign tumor of the hair follicle and scalp, with or without a history of previous trauma or inflammation to the area. It may also be genetically linked, which follows an autosomal dominant pattern although specific genes are not known.
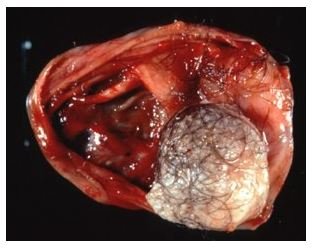
As the MPTT begins as a long standing benign tumor its appearance is that of a smooth, movable soft mass on the scalp with overlying hair loss. They may occur as single or multiple cysts and if inflamed, they may be red and tender to touch. Aside from the scalp, these tumors also grow in other places of the body like the neck, back, chest, buttock, arms, etc.
When the cysts suddenly become fast growing they are then considered proliferating trichilemmal tumors. They may start out to be well circumscribed, but as the growth increases the borders may be extended and poorly defined, and the mass becomes lobulated or irregular. Keratinization and calcification or hardening of the mass may be observed, and the tumor starts to invade connecting tissues. Metastasis or spread to distant sites of these cells may also occur.
Diagnosis is by biopsy and microscopic examination of the cells in the mass. The tumor should be distinguished from other forms of cancer of the skin and soft tissues.
Treatment of both benign and malignant tumors is by wide excision, and in the latter, a one centimeter margin of normal tissue around the mass must be excised. Chemotherapy and radiotherapy may be given in malignant cases. Long term follow-up must be done since local recurrences are known to occur . Patients must also be observed for metastases as the tumor cells are known to spread to distant sites, commonly involving the lymph nodes.