Find out how to test for osteochondroma using x-rays, CT scans, magnetic resonance imaging (MRI) and genetic tests.
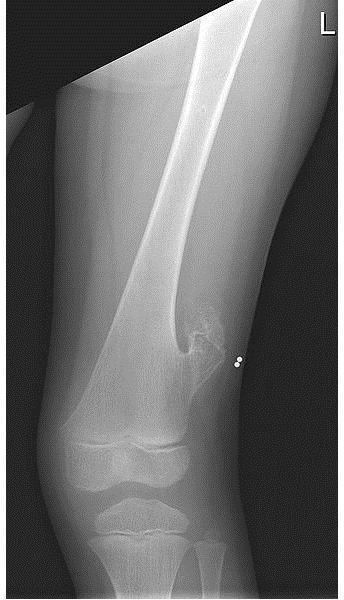
Previously referred to as osteocartilaginous exostosis, osteochondroma is a benign tumor usually occurring near the end of a long bone. The most common locations at which osteochondroma may be found include the distal femur and proximal tibia (around the knee joint) and the proximal humerus (near the shoulder)[1].
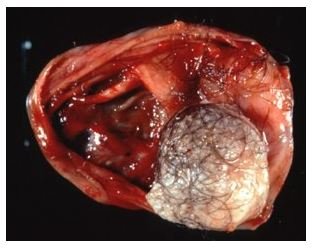
Osteochondromas are bony outgrowths with a cartilage cap and they usually appear between the ages of 10 and 30, when the bones are growing and maturing[2]. Osteochondroma may be asymptomatic, sufferers may report the existence of a hard, painless mass, or there may be pain caused by irritation to nearby muscles, tendons or nerves. Some patients may display slight angular deformities or limb length discrepancy[3].
Genetic and Non-inherited Forms of Osteochondroma
The cause of osteochondroma is not clearly understood, but there are two forms of the disease. Hereditary multiple osteochondromas is a genetic condition, and sufferers usually present with tumors in several locations. It is believed that the non-heritable form of the disease is caused by the detachment of a small piece of the bone growth plate during development[4].
Genetic Tests Can Be Used for Hereditary Multiple Osteochondromas
Hereditary multiple osteochondromas (HMO) are caused by mutations in a group of genes coding for exostosin (EXT) proteins. The mechanism by which the abnormal forms of the protein cause disease is not clearly understood. 90% of sufferers have inherited the faulty gene from their parents, and 10% suffer as a result of a new mutation. The disease is inherited in an autosomal dominant manner, meaning offspring of sufferers have a 50% chance of inheriting the disease.
Genetic tests involving sequence analysis of the relevant genes EXT-1 and EXT-2 are available. Mutations in EXT-1 account for between 56% and 78% of cases, with mutations in EXT-2 being present in 21% to 44% of cases[5].
Testing for Osteochondroma Involves Imaging Techniques
When considering how to test for osteochondroma it is worth bearing in mind that the condition is benign, and although some indications can be obtained from blood tests, the best way to confirm diagnosis is to use imaging techniques to identify abnormal bony or cartilaginous growths. Methods commonly used include x-rays, CT scans and MRI.
X-rays
X-rays use high frequency rays to penetrate the body and produce images of internal tissues. Bone and cartilage both absorb x-rays effectively so they can easily be seen on the resulting image. Osteochondroma can almost always be diagnosed using a simple x-ray, which will show the abnormal bony growth clearly[6].
Images
CT Scans
Computerised tomography scans (CT scans) use a combination of x-rays and computer technology to produce cross sectional images sometimes known as slices. CT scans can be used to distinguish between osteochondroma and chondrosarcoma, which is a malignant tumor appearing similar to osteochondroma on standard x-ray images[7].
MRI
Magnetic resonance imaging (MRI) is a valuable tool in the diagnosis and assessment of osteochondroma because it can provide detailed information about associated soft tissue pathology[8]. For example, an MRI scan can provide information about any compromise to blood vessels or compression of nerves caused by the growth. It can also be used to measure the thickness of the cartilage cap, a parameter which can be used to indicate whether the growth is benign or showing signs of developing into a malignant chondrosarcoma.
Citations
[1][3][6] “Osteochondroma ” Children’s Hospital Boston
[2][4] “Osteochondroma ” Medical University of South Carolina
[5] GA Schmale “Hereditary Multiple Osteochondromas ” Gene Reviews (1993)
[7] PJ Kenney, LA Gilula, WA Murphy “The Use of Computed Tomography to Distinguish Osteochondroma and Chondrosarcoma ” Radiology 139:129-137 (1981)
[8] K Woertler, N Linder, G Gosheger “Osteochondroma: MR Imaging of Tumor-Related Complications ” European Radiology 10:832-840 (1999)