The ependymoma of the filum terminale is located near the cauda equina, at the lower end of the spinal cord. It is an uncommon tumor, as ependymomas only represent 5 percent of all spinal tumors.
Introduction
Filum terminale ependymomas are growths inside of the lower part of the spinal cord. The growths are either benign or neoplastic (cancerous). Ependymomas are derived from the ependymal cells in the central nervous system, and are centrally located in the pia mater and spinal fluid. This pathology is also referred to myxopapillary ependymoma of the filum terminale. The term is synonymous due to the vast majority of filum terminale neoplasms are myxopapillary.
The classification is Latin-based. The suffix -oma refers to tumor. The filum terminale is loosely translated as “end thread” or “end filament”. Myx- is a mucous prefix, and papillary refers to tissue nipple-like in appearance.
Occurrence
Cancerous ependymomas of the filum terminale are common among children and the majority are benign. For benign tumors, the age of occurrence is 36 with male patients outnumbering female patients 2.2:1.
Reports indicate 1,126 ependymomas of the spinal cord per 100,000 people per year.
Symptoms and Diagnosis
Symptoms include sciatica or generalized lumbar pain. Sciatica refers to nerve pain radiating down the back of a patient’s leg. The pain can mimic a lumbar disc herniation. (6) When testing for generalized neurological symptoms, a dry spinal tap could indicate a filum terminale neoplasm.
Ependymomas of the filum terminale often have a diagnostic delay. The average delay from symptoms to diagnosis is roughly 50 months. Larger tumors, Grade 2, are discovered after an average of 17 months of symptoms. (5)
The hallmark sensation is lumbar pain; however, motor and sphincter dysfunction are less frequent symptoms.
Histopathology
The disease state requires invasive diagnostics such as biopsy to determine the exact type of growth. Radiographs are also used, which will be discussed later. Under the microscope, the cells appear radially arranged in a cube shape. As stated in the introduction, mucous-like liquid fills the spaces between the tumor cells. This patterning will appear around blood vessels, with possible basophils present. The tumor is propagated by stromal cells, a general term for immune cells. A test called GFAP is used to differentiate between tumors, and this type of tumor reacts to GFAP.
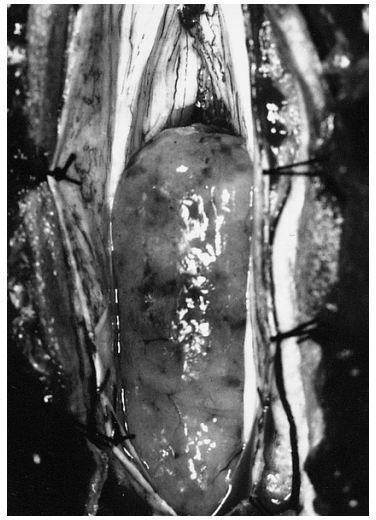
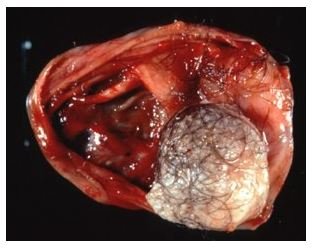
To the naked eye, the tumor will appear gray and separated into lobes.
Consider chordoma or schwannoma if spiral or spindle-shaped cells are not present.
Gross Section of a Filum Terminale Ependymoma
Radiology
Standard x-ray with contrast and magnetic resonance imaging (MRI) are available tools for recognizing ependymomas of the filum terminale. If highly suspected, these ependymomas cause obvious intensities. Specifically, isodense, or lighter than the surrounding spinal fluid. MRI should be completed with and without gadolinium contrast. Sagittal T1 and Sagittal T2 are the clearest views of the spinal pathology. (1,3)
Computed tomography is not recommended, as it does not pick up this type of tumor.
Treatment
Like most cancers, treatment is necessary to prevent spread (metastasis). Treatment for filum terminale ependymomas include surgery. The surgery calls for complete excision of the tumor. Radiograph follow-up is required to recognize tumor regrowth. In the unlikely event of metastasis, treatment includes radiation. (2)
References
- “Neoplasms of the Spinal Cord and Filum Terminale: Radiologic-Pathologic Correlation1.” RadioGraphics. Web. https://radiographics.rsna.org/content/20/6/1721/F12.expansion
- “Brain and Spinal Tumors: Hope Through Research.” National Institute of Neurological Disorders and Stroke (NINDS). Web. https://www.ninds.nih.gov/disorders/brainandspinaltumors/detail\_brainandspinaltumors.htm
- “Myxopapillary Ependymoma.” Neurowiki. Congress of Neurological Surgeons. Web. https://wiki.cns.org/wiki/index.php/Myxopapillary\_ependymoma
- Goldstein, Ira, et al. “Imaging in Spine Ependymoma.” Emedicine. Web. https://emedicine.medscape.com/article/345221-overview
- Byrne, Thomas N., Stephen G. Waxman, and Edward C. Benzel. Diseases of the Spine and Spinal Cord. Oxford: Oxford UP, 2000. Print.
- Menku, Ahmet, et al. “Ependymoma of Filum Terminale Mimicking Lumbar Disc Herniation.” Turkish Neurosurgery 14.3-4: 105-08. Web. https://neurosurgery.dergisi.org/pdf/pdf\_JTN\_21.pdf
- “Myxopapillary Ependymoma.” Histopathology-India.net. Web. https://www.histopathology-india.net/ME.htm