Primitive Neuroectodermal Tumor (PNET) is a rare form of brain tumor occurring usually in children below the age of 10. Survival rate is below 40 percent. Aggressive surgical resection, followed by chemotherapy and radiation therapy is recommended in most cases.
PNET Small Cell Brain Tumor
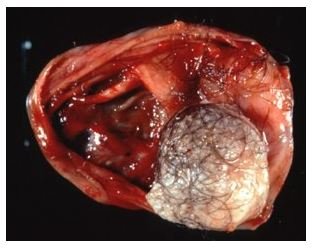
Primitive Neuroectodermal Tumor (PNET) is a soft tissue sarcoma of which medulloblastoma is the prototype. It is typically categorized under small round blue cell tumors (SRBCT). It is essentially a small cell, malignant embryonal tumor with varying differentiation along neural lines. It has several clinical and histological similarities with Ewing’s Sarcoma (ES), and a diagnostic distinction is made with advanced molecular biological analysis. PNET is primarily found in the upper thigh and hip region. In many cases it has an association with a large peripheral nerve such as the sciatic nerve.
PNET is a relatively rare, neural crest tumor. It usually occurs in children below the age of 10. The survival rate of this highly malignant tumor is under 40 percent. The tumor gets its name because a large number of cells in this tumor are a derivative of the neuroectoderm. These cells are under-developed and abnormal, which are termed as “primitive” cells. These primitive cells are believed to have been left over from the gestational development of the nervous system. In addition to the central nervous system, where this tumor is commonly located, it may also be found in the bone of the pelvis, the chest wall and the extremities.
Symptoms of Primitive Neuroectodermal Tumor
Typical symptoms of PNETs include general irritation and discomfort, vomiting and feeling of nausea, and a transient early morning headache or a headache that may disappear after vomiting. Other signs of the disease may be fatigue and body weakness, an unexplained change in sensation on one side of the body, seizures, longer sleep hours, weariness and draining of energy levels, sudden changes in behavior and personality, and unexplained weight gain or weight loss.
In an advanced stage of the disease, the symptoms may include poor sense of coordination causing difficulties in walking and balancing, double vision and dizziness. If these symptoms are noticed, it is important to get in touch with a physician for further examination. The physician will typically evaluate the physical condition and the past medical history and symptoms. Imaging analysis is the most crucial part in the diagnosis of this tumor, just like any other brain tumors.
Treatment of PNET
Treatment plan for this tumor will depend upon several factors such as the age of the patient, the general physical condition and medical history of the patient at the time of detection of the tumor. Other factors determining the initial treatment plan include the type, size and location of the tumor. Once the tumor has been surgically removed, some part of the tumor may still be left after the surgery. This will require a different treatment, just as if the tumor has spread beyond the the central nervous system to other parts of the body such as the lungs or bones.
Radiotherapy, surgery and chemotherapy are the key treatment options available to the operating team of doctors. In some cases, the doctors may also try to treat the disease by implanting a ventriculoperitoneal shunt. The aim of all these treatment options is to eliminate the maximum amount of tumor in order to restore CSF flow without causing neurological damage. The tumor may be highly aggressive and unpredictable, which makes some doctors recommend aggressive surgery followed by chemotherapy as well as radiotherapy.
Current Treatment Recommendations
The latest recommendations regarding treatment of PNETs and Ewing family of tumors include an aggressive surgical resection where possible, followed by adjuvant or neoadjuvant chemotherapy and radiation therapy. Multimodal treatment is advised so that the disease can be contained within the affected area, and chances of recurrence of the tumor are reduced. Similar treatment plan may also be followed for peripheral primitive neuroectodermal tumors (pPNETs).
References
https://emedicine.medscape.com/article/855644-overview