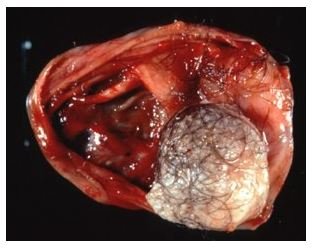
Mucinous pancreatic cyst neoplasm is a type of tumor of the pancreas with different degrees of malignancies. This disease appears mainly in women (95% of the cases). Learn about this disease and its treatment options.
Mucinous pancreatic cyst neoplasm occurs almost exclusively in women (95% of the reported cases) 40 to 50 years of age. The majority of these tumors are found in the tail of the pancreas. Mucinous cystic tumors are generally masses of 6-10 mm in size containing numerous fluid filled cavities called cysts. Mucinous cyst neoplasm of the pancreas has the following characteristics:
- they are not invasive of the large pancreatic ducts
- they make a sticky fluid called mucin (which fill the cysts) and
- they present a supporting structure called stroma.
The cysts sit on a structural supporting system (tissue) that resembles that of the female ovary (stroma). These tumors are classified according to the degree of dysplasia (dysplasia means abnormal form of the tissue) that they present in:
mucinous cystic neoplasms with low-grade dysplasia
mucinous cystic neoplasms with borderline malignant potential (with moderate dysplasia) and
Advertisementmucinous cystic neoplasms with high-grade dysplasia (carcinoma in situ).
Sign and Symptoms
Signs and symptoms of this type of disease are not very specific and can be similar to that of many diseases of the pancreas or even of other parts of the digestive system. In general, signs and symptoms of many pancreatic tumors include bloating, abdominal pain, unexplained weight loss, anorexia, and jaundice (if the tumor is located in the head of the pancreas).
Diagnosis
Imaging techniques are of paramount importance in diagnosing this disease. Ultrasound and computerized tomography will show specific traits of this type of tumor. Endoscopic ultrasound is more specific in detecting this type of tumor since it allows easier access to the pancreas and the possibility of taking samples for histological (tissue) analysis. Certain markers of the mucinous pancreatic cyst neoplasm can be evaluated in the patient’s blood such as the CEA tumor marker which in 79% of the cases may have validity but is not correlated with the malignancy of the tumor.
Treatment
The best treatment for mucinous cystic neoplasms is complete surgical removal even if the tumor is benign. For patients with surgical risks there is an alternative therapy under research consisting of injection of ethanol and taxol (a potent cancer killing agent) directly inside the pancreatic parenchyma. However, the best treatment is surgical removal since the tumor will likely have an evolution towards malignancy and no efficacy has been shown with chemotherapy or radiation therapy.
References:
What are pancreatic tumors? John Hopkins University (https://pathology.jhu.edu/pancreas/BasicTypes2.php#mucin )
Catalano et al. Mucinous cystic neoplasm of the pancreas. Chirurgia Italiana 2009 - vol. 61 n. 3 pp 375-379 (https://www.sichirurgia.org/editoria/rivista/2009/N3_2009/PDF/Catalano_309.pdf )
Goh BK, Tan YM, Chung YF, Chow PK, Cheow PC, Wong WK, Ooi LL. A review of mucinous cystic neoplasms of the pancreas defined by ovarian-type stroma: clinico pathological features of 344 patients. World J Surg 2006; 30: 2236 - 45.