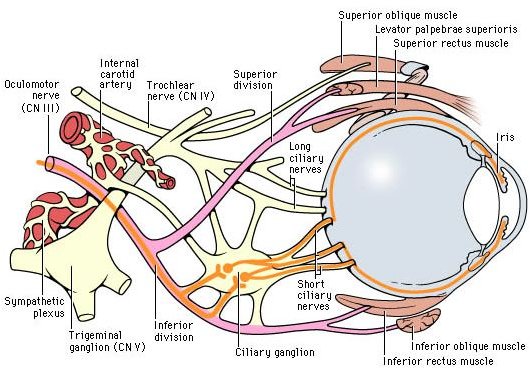
The oculomotor nerve, or cranial nerve III, is the major workhorse of eye movement, and is central to movement of the eye, eyelid, and pupil. Learn about this important nerve that enables proper movement of your eye.
Oculomotor Nerve Function
The oculomotor nerve is also known as cranial nerve (CN) III. The oculomotor nerve innervates many of the muscles responsible for eye movement. Two other cranial nerves also contribute to eye movement: the trochlear never (CN IV) and the abducens nerve (CN VI), but the oculomotor nerve is responsible for the majority of eye movement. In addition to motor fibers, the oculomotor nerve also contain parasympathetic nerve fibers. The parasympathetic functions of the oculomotor nerve include keeping the eyelid open and maintaining the pupillary reflex to light. The oculomotor nerve does not carry sensory fibers and is not responsible for vision (this function is controlled by the optic nerve: cranial nerve II).
Oculomotor Nerve Connections
Like other cranial nerves, the oculomotor nerve originates in the brainstem. Specifically, the oculomotor nerve originates in the midbrain between the cerebral peduncles. The oculomotor nerve enters the orbit (eye socket) through an opening known as the superior orbital fissure. The oculomotor nerve sends fibers to several muscles of the eye, including the inferior oblique, the superior rectus, the medial rectus, and the inferior rectus muscles to control eye movements. The parasympethics fibers of the oculomotor nerve arise from the Edinger-Westphal nucleus, and pass through the ciliary ganglion to connect to the levator palpebrae superioris muscle of the eyelid, the sphincter muscle of the iris, and the ciliary muscle within the pupil.
The Oculomotor Nerve
Oculomotor Nerve Palsy
If the oculomotor nerve is damaged or otherwise not functioning properly, eye movement is severely impaired. Physicians describe the appearance of a paralyzed oculomotor nerve (known as palsy) as “down and out,” indicating the position of the patient’s eyes. Additionally, the eyelid may droop and the pupils may fail to react to light, due to damage of parasympathetic fibers. The presentation of an oculomotor nerve palsy depends on which part of the nerve is damaged. Though oculomotor nerve palsy is rare, it may be seen in people with direct eye trauma, ischemia (which can be caused by advanced diabetes), aneurysm, or intracranial tumors, among other causes.
References
Dhillon, N. “Anatomy: Cranial Nerves” Current Diagnosis &T reatment in Otalaryngology. McGraw-Hill, 2008.
Galvin, J. “Mental Status and neurological Examination in Older Adults.” Hazzard’s Geriatric Medicine and Gerontology, 6th Ed. McGraw-Hill, 2009.
Riordan-Eva P, Hoyt W. “Neuro-Ophthalmology.” Vaughan & Asbury’s General Ophthalmology, 17th Ed. McGraw-Hill, 2009.
Image Credit
Yale University School of Medicine. https://www.med.yale.edu/caim/cnerves/cn3/cn3 _graphics/cn3_1.jpg