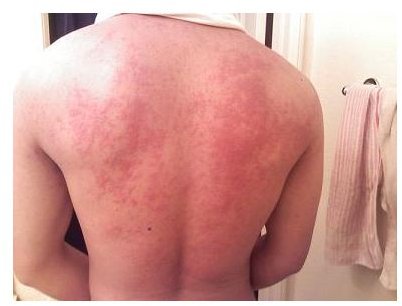
Urticaria is a type of skin disorder in which the skin becomes red and inflamed. In urticarial vasculitis, blood vessels are also affected.
What is Urticaria?
Urticaria skin disorders cause reddened patches and wheals to form on the skin. Wheals are swollen patches of skin, which can vary in size from a few millimeters in diameter to several inches. In severe cases wheals may cover very large areas of skin, such as the chest or back. Wheals are patchy in color, with areas of pale and reddened skin. They are often itchy.
Urticaria develops when immune cells called mast cells release chemicals in the skin. These chemicals, which include histamines, cause blood vessels in the skin to become leaky, allowing excess fluid to seep into the skin. The excess fluid leads to swelling, and the chemicals can cause skin itching.
In urticarial vasculitis, blood vessels become inflamed in addition to skin inflammation.
Signs and Symptoms of Urticarial Vasculitis
The first sign of urticaria vasculitis is painful, burning urticaria lesions. These painful sensations indicate that blood vessels are becoming inflamed. If itching is present it can become more severe as the inflammation worsens.
Vasculitis lesions are reddish in color, and are often pale in the center. There might be small spots of blood called petechiae under the skin.
These lesions might remain for 24 hours or longer before they begin to heal. As the lesions heal they can begin to resemble bruises, with the skin becoming darker before returning to its normal color.
Some people develop other symptoms in addition to skin lesions. Possible symptoms include sensitivity to light, swollen lymph nodes, fever, joint pain, abdominal pain, and breathing difficulty. More rarely, lung or kidney problems can develop.
Causes and Risk Factors
In most cases, urticaria vasculitis is idiopathic, which means it has no known cause.
In some cases, however, this condition is associated with certain disorders of the immune system. These include the inflammatory connective tissue disorders such as Sjorgen syndrome and systemic lupus erythematosus, immunoglobulin disorders, and leukemia.
Certain viral diseases, including hepatitis B and hepatitis C, and infectious mononucleosis, are also associated with this type of vasculitis.
In addition, there are some medication types that can increase the risk in some people. These include penicillin, ACE inhibitors, the antidepressant fluoexetine (Prozac), and thiazide diuretics.
Treatment Options
Most people with this skin condition have a good prognosis, although healing is often slow. It is common for treatment to help resolve the condition within months, or occasionally a year or longer. In some cases, the disease may become chronic, requiring long-term treatment to manage the symptoms. This skin condition is only dangerous or life-threatening in cases where kidney or lung problems develop as a result of systemic disease.
Treatment is usually based on how long the vasculitis lesions have been active, and whether the lesions are painful, burning, or itchy.
Most patients will consult with a dermatologist to confirm the diagnosis and determine the best course of treatment. Alternatively, a biopsy is taken of a skin lesion, and this skin sample is examined by a dermatologist. Patients might see other specialists depending on their individual situation; someone with lupus might see a rheumatologist, while someone with allergic urticaria might see an allergist or clinical immunologist.
Common medications include antihistamines and non-steroidal anti-inflammatory drugs, which are prescribed for people who have only mild to moderate skin lesions, with no involvement of other organs or body systems. People with more severe disease might be prescribed a short to medium course of corticosteroids to suppress the inflammation.
References
Darius Mehregan, MD, for eMedicine: Diseases of the Vessels: Urticarial Vasculitis
Kjetil Kristoffer Guldbakke, MD and Amor Khachemoune, MD, CWS for eMedicine: Classification and Treatment of Urticaria: A Brief Review