Learn about the use of bone marrow transplants for non-Hodgkins lymphoma, including why bone marrow transplants are needed, what the procedures involve and the potential risks
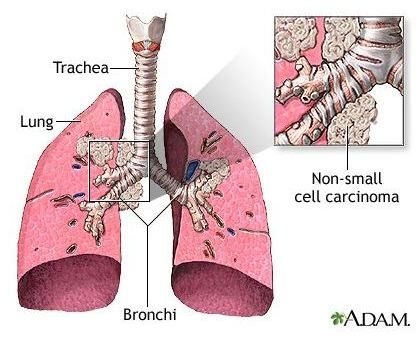
Non-Hodgkin’s lymphoma is a cancer of the lymphatic system, which is a series of nodes and glands forming an important part of the body’s immune system. Tissue fluid from different parts of the body drains into the lymphatic system, which contains large numbers of lymphocytes (a type of white blood cell). The lymphocytes identify and destroy any foreign cells or material before the fluid is returned to the blood.
What is Non-Hodgkin’s Lymphoma?
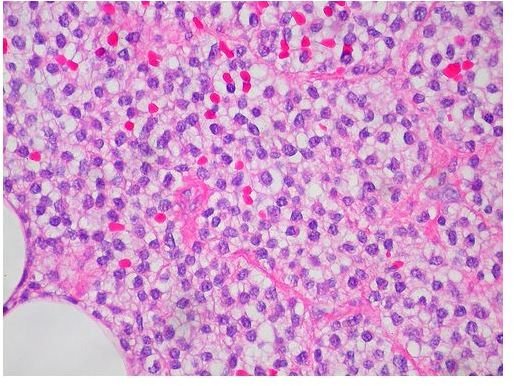
In lymphoma, the lymphocytes begin to multiply abnormally and lose their ability to fight infection. They collect in the lymph nodes causing swelling, and may spill out into the blood stream as well, infecting other parts of the body. Most of the symptoms of lymphoma are due to the body’s reduced capacity to fight infection. Non-Hodgkin’s lymphoma is the most common form of lymphoma, occurring more frequently in older patients, and lacking the distinctive Reed-Sternberg cells found in Hodgkin’s lymphoma.
Abnormal Lymphocytes in Lymphoma
Why Use Bone Marrow Transplant for Non-Hodgkin’s Lymphoma?
Non-Hodgkin’s lymphoma is usually treated by destroying the cancerous cells using aggressive chemotherapy techniques. However, this therapy can damage the bone marrow of the patient. Bone marrow contains hematopoietic stem cells which give rise to components of blood including red and white blood cells and platelets. Chemotherapy can leave non-Hodgkins lymphoma patients unable to manufacture sufficient new blood components in order to aid their recovery.
To enable the patient to recover well from their course of chemotherapy, doctors may decide to harvest healthy bone marrow prior to the treatment and replace it after the chemotherapy is complete. This is known as an autologous transplant, meaning the patient receives a graft of their own body tissue.
What is the Procedure for Bone Marrow Transplant?
The bone marrow harvest takes place under general anesthetic before chemotherapy begins. The doctors remove the bone marrow using a needle which is usually inserted into the hip bone. Several different locations are normally needed to ensure sufficient bone marrow is harvested. About two pints of bone marrow are removed and frozen. After the harvest, patients will usually feel sore and bruised for up to a week, and some patients will need a blood transfusion.
After the course of chemotherapy treatment, the bone marrow is returned to the patient’s body via an intra-venous drip. The bone marrow stem cells then migrate to the large bones of the body and resume their function giving rise to components of blood.
If autologous transplant is not possible, patients may be given a bone marrow transplant from a donor with a suitably-matched tissue type. Some patients may be given umbilical cord stem cells from a stem cell bank as an alternative, in particular if they have a rare tissue type, as cord stem cells do not need to be so closely matched.
What Are the Risks of the Transplant?
The risks and side effects of the procedure depend on whether the transplant was autologous or came from a donor. With any type of bone marrow transplant, patients may suffer side effects of anaemia, risk of infection, bleeding or mucositis (inflammation of the mucous membranes). There is a risk that the transplant cells may not migrate to the bone marrow successfully, in which case the procedure may need to be repeated. If the transplant came from a donor, there is a small risk of developing graft versus host disease (GVHD) in which the grafted cells begin to attack the patient’s own healthy cells.
Citations
[1] “Adult Non-Hodgkin Lymphoma Treatment ” National Cancer Institute website
[2] “Lymphoma ” NHS Choices website
[3][4][5] “Bone Marrow Transplants for Non-Hodgkin’s Lymphoma ” Cancer Research UK website
[6] V Rocha, M Labopin, G Sanz “Transplants of Umbilical Cord Blood or Bone Marrow From Unrelated Donors in Adults with Acute Leukemia ” New England Journal of Medicine 352:935-937 (2005)
[7] “Bone Marrow (Stem Cell) Transplantation ” BUPA factsheet
Image courtesy of Ed Uthmann