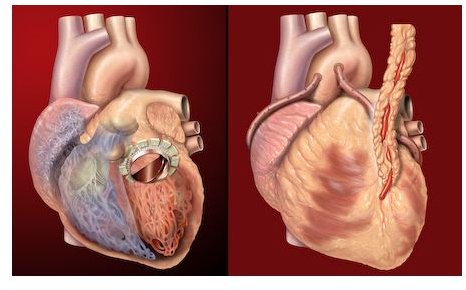
Learn about what happens during a myocardial infarction. How is the blood flow to the heart stopped, and what causes it?
About Myocardial Infarction
Myocardial infarction (MI), commonly known as heart attack, is the leading cause of death across the globe, yet not many people know what happens during a myocardial infarction. The short answer is that oxygenated blood does not reach the heart muscle. However, there are a few different mechanisms of this lack of blood supply (ischemia). Myocardial infarctions can be categorized as transmural or nontransmural. Transmural infarctions affect the cells all the way through the heart wall; they affect cells on the inside of the heart (endocardium), the central, muscular layer (myocardium) and the external layer of the heart (epicardium). Nontransmural MI affects either the endocardium or both the endocardium and myocardium; they do not generally affect the epicardium.
Advances in medical technology and treatment options have improved the survival rates of patients hospitalized presenting with MI to 95 percent. Most MIs occur in patients over 65 years of age, advanced age being a major risk factor. Other risk factors include high blood lipid levels (hyperlipidemia), diabetes mellitus, high blood pressure (hypertension), male gender, tobacco use and family history. These risk factors increase the likelihood that a patient will develop fatty deposits (atherosclerotic plaques) on the walls of the arteries that supply the heart with blood (coronary arteries).
Unstable Atherosclerosis
Most MIs occur as a result of an unstable atherosclerotic plaque in one or more of the coronary arteries. The atherosclerotic plaques develop over long periods of time. As they grow, they become unstable and may rupture. Ruptured plaques expose the components that make up the plaque including collagen. The collagen begins to collect platelets—cell fragments present in the blood stream—and, coupled with the release of several enzymes, two dangerous reactions occur at the site of the ruptured plaque. A blood clot (called a thrombus when it occurs inside a blood vessel) forms, and the artery constricts, both as a result of the enzymes and due to the damage to the inner layer of the blood vessel (endothelium).
As the thrombus grows, it begins to occlude and eventually completely block the now narrowed blood vessel. This causes a few different effects in the function of the heart. The heart must now pump harder and faster to maintain proper blood flow. This dangerously increases blood pressure and resting heart rate. The cellular metabolic requirements of oxygen and nutrients are now not being met distal to the thrombus. The cells that are not receiving blood begin to die due to lack of oxygen and nutrients. The ability of the muscle in the affected area to contract is diminished almost immediately following the onset of ischemia.
If the thrombus is cleared and blood flow resumes (reperfusion), the muscle cells may recover. Irreversible damage to the heart muscle occurs within 20 minutes of ischemia.
Metabolic Insufficiency
Another cause of MI, and sometimes triggering ischemia from unstable atherosclerosis, is situations that increase the metabolic needs of the heart without being met. These include emotional stress or extreme physical activity. This often occurs in conjunction with atherosclerosis. As the plaques grow, the hollow space (lumen) of the coronary arteries is diminished. This slows blood flow and decreases the amount of blood reaching the heart tissues. During situations that cause the heart rate to increase, the heart cells require more oxygen to continue supplying the rest of the body with oxygenated blood. The occluded lumen of the arteries restricts blood flow, and the heart muscle cells undergo ischemia and begin to die (infarct).
References
Cleveland Clinic: Acute Myocardial Infarction
Blackwell Publishing: Sample of Aaronson-Pathophysiology of Acute Myocardial Infarction
National Heart Lung and Blood Institute: What Is A Heart Attack?